What Is Schizophrenia?
Schizophrenia is a chronic, severe, and disabling brain disorder that has affected people throughout history.
People with the disorder may hear voices other people don't hear. They may believe other people are reading their minds, controlling their thoughts, or plotting to harm them. This can terrify people with the illness and make them withdrawn or extremely agitated.
People with schizophrenia may not make sense when they talk. They may sit for hours without moving or talking. Sometimes people with schizophrenia seem perfectly fine until they talk about what they are really thinking.
Families and society are affected by schizophrenia too. Many people with schizophrenia have difficulty holding a job or caring for themselves, so they rely on others for help.
Treatment helps relieve many symptoms of schizophrenia, but most people who have the disorder cope with symptoms throughout their lives. However, many people with schizophrenia can lead rewarding and meaningful lives in their communities. Researchers are developing more effective medications and using new research tools to understand the causes of schizophrenia. In the years to come, this work may help prevent and better treat the illness.
Causes
Experts think schizophrenia is caused by several factors.
Genes and environment. Scientists have long known that schizophrenia runs in families. The illness occurs in 1 percent of the general population, but it occurs in 10 percent of people who have a first-degree relative with the disorder, such as a parent, brother, or sister. People who have second-degree relatives (aunts, uncles, grandparents, or cousins) with the disease also develop schizophrenia more often than the general population. The risk is highest for an identical twin of a person with schizophrenia. He or she has a 40 to 65 percent chance of developing the disorder.
We inherit our genes from both parents. Scientists believe several genes are associated with an increased risk of schizophrenia, but that no gene causes the disease by itself. In fact, recent research has found that people with schizophrenia tend to have higher rates of rare genetic mutations. These genetic differences involve hundreds of different genes and probably disrupt brain development.
Other recent studies suggest that schizophrenia may result in part when a certain gene that is key to making important brain chemicals malfunctions. This problem may affect the part of the brain involved in developing higher functioning skills. Research into this gene is ongoing, so it is not yet possible to use the genetic information to predict who will develop the disease.
Despite this, tests that scan a person's genes can be bought without a prescription or a health professional's advice. Ads for the tests suggest that with a saliva sample, a company can determine if a client is at risk for developing specific diseases, including schizophrenia. However, scientists don't yet know all of the gene variations that contribute to schizophrenia. Those that are known raise the risk only by very small amounts. Therefore, these "genome scans" are unlikely to provide a complete picture of a person's risk for developing a mental disorder like schizophrenia.
In addition, it probably takes more than genes to cause the disorder. Scientists think interactions between genes and the environment are necessary for schizophrenia to develop. Many environmental factors may be involved, such as exposure to viruses or malnutrition before birth, problems during birth, and other not yet known psychosocial factors.
Different brain chemistry and structure. Scientists think that an imbalance in the complex, interrelated chemical reactions of the brain involving the neurotransmitters dopamine and glutamate, and possibly others, plays a role in schizophrenia. Neurotransmitters are substances that allow brain cells to communicate with each other. Scientists are learning more about brain chemistry and its link to schizophrenia.
Also, in small ways the brains of people with schizophrenia look different than those of healthy people. For example, fluid-filled cavities at the center of the brain, called ventricles, are larger in some people with schizophrenia. The brains of people with the illness also tend to have less gray matter, and some areas of the brain may have less or more activity.
Studies of brain tissue after death also have revealed differences in the brains of people with schizophrenia. Scientists found small changes in the distribution or characteristics of brain cells that likely occurred before birth. Some experts think problems during brain development before birth may lead to faulty connections. The problem may not show up in a person until puberty. The brain undergoes major changes during puberty, and these changes could trigger psychotic symptoms. Scientists have learned a lot about schizophrenia, but more research is needed to help explain how it develops.
Who Is At Risk?
About 1% of Americans have this illness.
Schizophrenia affects men and women equally. It occurs at similar rates in all ethnic groups around the world. Symptoms such as hallucinations and delusions usually start between ages 16 and 30. Men tend to experience symptoms a little earlier than women. Most of the time, people do not get schizophrenia after age 45. Schizophrenia rarely occurs in children, but awareness of childhood-onset schizophrenia is increasing.
It can be difficult to diagnose schizophrenia in teens. This is because the first signs can include a change of friends, a drop in grades, sleep problems, and irritability—behaviors that are common among teens. A combination of factors can predict schizophrenia in up to 80% of youth who are at high risk of developing the illness. These factors include isolating oneself and withdrawing from others, an increase in unusual thoughts and suspicions, and a family history of psychosis. In young people who develop the disease, this stage of the disorder is called the "prodromal" period.
Signs & Symptoms
The symptoms of schizophrenia fall into three broad categories: positive symptoms, negative symptoms, and cognitive symptoms.
Positive symptoms
Positive symptoms are psychotic behaviors not seen in healthy people. People with positive symptoms often "lose touch" with reality. These symptoms can come and go. Sometimes they are severe and at other times hardly noticeable, depending on whether the individual is receiving treatment. They include the following:
Hallucinations are things a person sees, hears, smells, or feels that no one else can see, hear, smell, or feel. "Voices" are the most common type of hallucination in schizophrenia. Many people with the disorder hear voices. The voices may talk to the person about his or her behavior, order the person to do things, or warn the person of danger. Sometimes the voices talk to each other. People with schizophrenia may hear voices for a long time before family and friends notice the problem.
Other types of hallucinations include seeing people or objects that are not there, smelling odors that no one else detects, and feeling things like invisible fingers touching their bodies when no one is near.
Delusions are false beliefs that are not part of the person's culture and do not change. The person believes delusions even after other people prove that the beliefs are not true or logical. People with schizophrenia can have delusions that seem bizarre, such as believing that neighbors can control their behavior with magnetic waves. They may also believe that people on television are directing special messages to them, or that radio stations are broadcasting their thoughts aloud to others. Sometimes they believe they are someone else, such as a famous historical figure. They may have paranoid delusions and believe that others are trying to harm them, such as by cheating, harassing, poisoning, spying on, or plotting against them or the people they care about. These beliefs are called "delusions of persecution."
Thought disorders are unusual or dysfunctional ways of thinking. One form of thought disorder is called "disorganized thinking." This is when a person has trouble organizing his or her thoughts or connecting them logically. They may talk in a garbled way that is hard to understand. Another form is called "thought blocking." This is when a person stops speaking abruptly in the middle of a thought. When asked why he or she stopped talking, the person may say that it felt as if the thought had been taken out of his or her head. Finally, a person with a thought disorder might make up meaningless words, or "neologisms."
Movement disorders may appear as agitated body movements. A person with a movement disorder may repeat certain motions over and over. In the other extreme, a person may become catatonic. Catatonia is a state in which a person does not move and does not respond to others. Catatonia is rare today, but it was more common when treatment for schizophrenia was not available.
Negative symptoms
Negative symptoms are associated with disruptions to normal emotions and behaviors. These symptoms are harder to recognize as part of the disorder and can be mistaken for depression or other conditions. These symptoms include the following:
- "Flat affect" (a person's face does not move or he or she talks in a dull or monotonous voice)
- Lack of pleasure in everyday life
- Lack of ability to begin and sustain planned activities
- Speaking little, even when forced to interact.
People with negative symptoms need help with everyday tasks. They often neglect basic personal hygiene. This may make them seem lazy or unwilling to help themselves, but the problems are symptoms caused by the schizophrenia.
Cognitive symptoms
Cognitive symptoms are subtle. Like negative symptoms, cognitive symptoms may be difficult to recognize as part of the disorder. Often, they are detected only when other tests are performed. Cognitive symptoms include the following:
- Poor "executive functioning" (the ability to understand information and use it to make decisions)
- Trouble focusing or paying attention
- Problems with "working memory" (the ability to use information immediately after learning it).
Cognitive symptoms often make it hard to lead a normal life and earn a living. They can cause great emotional distress.
Treatments
Because the causes of schizophrenia are still unknown, treatments focus on eliminating the symptoms of the disease. Treatments include antipsychotic medications and various psychosocial treatments.
Antipsychotic medications
Antipsychotic medications have been available since the mid-1950's. The older types are called conventional or "typical" antipsychotics. Some of the more commonly used typical medications include:
- Chlorpromazine (Thorazine)
- Haloperidol (Haldol)
- Perphenazine (Etrafon, Trilafon)
- Fluphenazine (Prolixin).
In the 1990's, new antipsychotic medications were developed. These new medications are called second generation, or "atypical" antipsychotics.
One of these medications, clozapine (Clozaril) is an effective medication that treats psychotic symptoms, hallucinations, and breaks with reality. But clozapine can sometimes cause a serious problem called agranulocytosis, which is a loss of the white blood cells that help a person fight infection. People who take clozapine must get their white blood cell counts checked every week or two. This problem and the cost of blood tests make treatment with clozapine difficult for many people. But clozapine is potentially helpful for people who do not respond to other antipsychotic medications.
Other atypical antipsychotics were also developed. None cause agranulocytosis. Examples include:
- Risperidone (Risperdal)
- Olanzapine (Zyprexa)
- Quetiapine (Seroquel)
- Ziprasidone (Geodon)
- Aripiprazole (Abilify)
- Paliperidone (Invega).
What are the side effects?
Some people have side effects when they start taking these medications. Most side effects go away after a few days and often can be managed successfully. People who are taking antipsychotics should not drive until they adjust to their new medication. Side effects of many antipsychotics include:
- Drowsiness
- Dizziness when changing positions
- Blurred vision
- Rapid heartbeat
- Sensitivity to the sun
- Skin rashes
- Menstrual problems for women.
Atypical antipsychotic medications can cause major weight gain and changes in a person's metabolism. This may increase a person's risk of getting diabetes and high cholesterol. A person's weight, glucose levels, and lipid levels should be monitored regularly by a doctor while taking an atypical antipsychotic medication.
Typical antipsychotic medications can cause side effects related to physical movement, such as:
- Rigidity
- Persistent muscle spasms
- Tremors
- Restlessness.
Long-term use of typical antipsychotic medications may lead to a condition called tardive dyskinesia (TD). TD causes muscle movements a person can't control. The movements commonly happen around the mouth. TD can range from mild to severe, and in some people the problem cannot be cured. Sometimes people with TD recover partially or fully after they stop taking the medication.
TD happens to fewer people who take the atypical antipsychotics, but some people may still get TD. People who think that they might have TD should check with their doctor before stopping their medication.
How are antipsychotics taken and how do people respond to them?
Antipsychotics are usually in pill or liquid form. Some anti-psychotics are shots that are given once or twice a month.
Symptoms of schizophrenia, such as feeling agitated and having hallucinations, usually go away within days. Symptoms like delusions usually go away within a few weeks. After about six weeks, many people will see a lot of improvement.
However, people respond in different ways to antipsychotic medications, and no one can tell beforehand how a person will respond. Sometimes a person needs to try several medications before finding the right one. Doctors and patients can work together to find the best medication or medication combination, as well as the right dose.
Some people may have a relapse-their symptoms come back or get worse. Usually, relapses happen when people stop taking their medication, or when they only take it sometimes. Some people stop taking the medication because they feel better or they may feel they don't need it anymore. But no one should stop taking an antipsychotic medication without talking to his or her doctor. When a doctor says it is okay to stop taking a medication, it should be gradually tapered off, never stopped suddenly.
How do antipsychotics interact with other medications?
Antipsychotics can produce unpleasant or dangerous side effects when taken with certain medications. For this reason, all doctors treating a patient need to be aware of all the medications that person is taking. Doctors need to know about prescription and over-the-counter medicine, vitamins, minerals, and herbal supplements. People also need to discuss any alcohol or other drug use with their doctor.
To find out more about how antipsychotics work, the National Institute of Mental Health (NIMH) funded a study called CATIE (Clinical Antipsychotic Trials of Intervention Effectiveness). This study compared the effectiveness and side effects of five antipsychotics used to treat people with schizophrenia. In general, the study found that the older typical antipsychotic perphenazine (Trilafon) worked as well as the newer, atypical medications. But because people respond differently to different medications, it is important that treatments be designed carefully for each person. More information about CATIE is on the NIMH website.
Psychosocial treatments
Psychosocial treatments can help people with schizophrenia who are already stabilized on antipsychotic medication. Psychosocial treatments help these patients deal with the everyday challenges of the illness, such as difficulty with communication, self-care, work, and forming and keeping relationships. Learning and using coping mechanisms to address these problems allow people with schizophrenia to socialize and attend school and work.
Patients who receive regular psychosocial treatment also are more likely to keep taking their medication, and they are less likely to have relapses or be hospitalized. A therapist can help patients better understand and adjust to living with schizophrenia. The therapist can provide education about the disorder, common symptoms or problems patients may experience, and the importance of staying on medications. For more information on psychosocial treatments, see the psychotherapies section on the NIMH website.
Illness management skills. People with schizophrenia can take an active role in managing their own illness. Once patients learn basic facts about schizophrenia and its treatment, they can make informed decisions about their care. If they know how to watch for the early warning signs of relapse and make a plan to respond, patients can learn to prevent relapses. Patients can also use coping skills to deal with persistent symptoms.
Integrated treatment for co-occurring substance abuse. Substance abuse is the most common co-occurring disorder in people with schizophrenia. But ordinary substance abuse treatment programs usually do not address this population's special needs. When schizophrenia treatment programs and drug treatment programs are used together, patients get better results.
Rehabilitation. Rehabilitation emphasizes social and vocational training to help people with schizophrenia function better in their communities. Because schizophrenia usually develops in people during the critical career-forming years of life (ages 18 to 35), and because the disease makes normal thinking and functioning difficult, most patients do not receive training in the skills needed for a job.
Rehabilitation programs can include job counseling and training, money management counseling, help in learning to use public transportation, and opportunities to practice communication skills. Rehabilitation programs work well when they include both job training and specific therapy designed to improve cognitive or thinking skills. Programs like this help patients hold jobs, remember important details, and improve their functioning.
Family education. People with schizophrenia are often discharged from the hospital into the care of their families. So it is important that family members know as much as possible about the disease. With the help of a therapist, family members can learn coping strategies and problem-solving skills. In this way the family can help make sure their loved one sticks with treatment and stays on his or her medication. Families should learn where to find outpatient and family services.
Cognitive behavioral therapy. Cognitive behavioral therapy (CBT) is a type of psychotherapy that focuses on thinking and behavior. CBT helps patients with symptoms that do not go away even when they take medication. The therapist teaches people with schizophrenia how to test the reality of their thoughts and perceptions, how to "not listen" to their voices, and how to manage their symptoms overall. CBT can help reduce the severity of symptoms and reduce the risk of relapse.
Self-help groups. Self-help groups for people with schizophrenia and their families are becoming more common. Professional therapists usually are not involved, but group members support and comfort each other. People in self-help groups know that others are facing the same problems, which can help everyone feel less isolated. The networking that takes place in self-help groups can also prompt families to work together to advocate for research and more hospital and community treatment programs. Also, groups may be able to draw public attention to the discrimination many people with mental illnesses face.
Living With
How can you help a person with schizophrenia?
People with schizophrenia can get help from professional case managers and caregivers at residential or day programs. However, family members usually are a patient's primary caregivers.
People with schizophrenia often resist treatment. They may not think they need help because they believe their delusions or hallucinations are real. In these cases, family and friends may need to take action to keep their loved one safe. Laws vary from state to state, and it can be difficult to force a person with a mental disorder into treatment or hospitalization. But when a person becomes dangerous to himself or herself, or to others, family members or friends may have to call the police to take their loved one to the hospital.
Treatment at the hospital. In the emergency room, a mental health professional will assess the patient and determine whether a voluntary or involuntary admission is needed. For a person to be admitted involuntarily, the law states that the professional must witness psychotic behavior and hear the person voice delusional thoughts. Family and friends can provide needed information to help a mental health professional make a decision.
After a loved one leaves the hospital. Family and friends can help their loved ones get treatment and take their medication once they go home. If patients stop taking their medication or stop going to follow-up appointments, their symptoms likely will return. Sometimes symptoms become severe for people who stop their medication and treatment. This is dangerous, since they may become unable to care for themselves. Some people end up on the street or in jail, where they rarely receive the kind of help they need.
Family and friends can also help patients set realistic goals and learn to function in the world. Each step toward these goals should be small and taken one at a time. The patient will need support during this time. When people with a mental illness are pressured and criticized, they usually do not get well. Often, their symptoms may get worse. Telling them when they are doing something right is the best way to help them move forward.
It can be difficult to know how to respond to someone with schizophrenia who makes strange or clearly false statements. Remember that these beliefs or hallucinations seem very real to the person. It is not helpful to say they are wrong or imaginary. But going along with the delusions is not helpful, either. Instead, calmly say that you see things differently. Tell them that you acknowledge that everyone has the right to see things his or her own way. In addition, it is important to understand that schizophrenia is a biological illness. Being respectful, supportive, and kind without tolerating dangerous or inappropriate behavior is the best way to approach people with this disorder.
Are people with schizophrenia violent?
People with schizophrenia are not usually violent. In fact, most violent crimes are not committed by people with schizophrenia. However, some symptoms are associated with violence, such as delusions of persecution. Substance abuse may also increase the chance a person will become violent. If a person with schizophrenia becomes violent, the violence is usually directed at family members and tends to take place at home.
The risk of violence among people with schizophrenia is small. But people with the illness attempt suicide much more often than others. About 10 percent (especially young adult males) die by suicide. It is hard to predict which people with schizophrenia are prone to suicide. If you know someone who talks about or attempts suicide, help him or her find professional help right away.
What about substance abuse?
Some people who abuse drugs show symptoms similar to those of schizophrenia. Therefore, people with schizophrenia may be mistaken for people who are affected by drugs. Most researchers do not believe that substance abuse causes schizophrenia. However, people who have schizophrenia are much more likely to have a substance or alcohol abuse problem than the general population.
Substance abuse can make treatment for schizophrenia less effective. Some drugs, like marijuana and stimulants such as amphetamines or cocaine, may make symptoms worse. In fact, research has found increasing evidence of a link between marijuana and schizophrenia symptoms. In addition, people who abuse drugs are less likely to follow their treatment plan.
Schizophrenia and smoking
Addiction to nicotine is the most common form of substance abuse in people with schizophrenia. They are addicted to nicotine at three times the rate of the general population (75 to 90 percent vs. 25 to 30 percent).
The relationship between smoking and schizophrenia is complex. People with schizophrenia seem to be driven to smoke, and researchers are exploring whether there is a biological basis for this need. In addition to its known health hazards, several studies have found that smoking may make antipsychotic drugs less effective.
Quitting smoking may be very difficult for people with schizophrenia because nicotine withdrawal may cause their psychotic symptoms to get worse for a while. Quitting strategies that include nicotine replacement methods may be easier for patients to handle. Doctors who treat people with schizophrenia should watch their patients' response to antipsychotic medication carefully if the patient decides to start or stop smoking.
-----------------------------------------------------------------------------------------------------------------------------
Schizophrenia is a psychiatric diagnosis that describes a mental disorder characterized by abnormalities in the perception or expression of reality. Distortions in perception may affect all five senses, including sight, hearing, taste, smell and touch, but most commonly manifest as auditory hallucinations, paranoid or bizarre delusions, or disorganized speech and thinking with significant social or occupational dysfunction. Onset of symptoms typically occurs in young adulthood, with approximately 0.4–0.6% of the population affected. Diagnosis is based on the patient's self-reported experiences and observed behavior. No laboratory test for schizophrenia currently exists.
Studies suggest that genetics, early environment, neurobiology, psychological and social processes are important contributory factors; some recreational and prescription drugs appear to cause or worsen symptoms. Current psychiatric research is focused on the role of neurobiology, but no single organic cause has been found. As a result of the many possible combinations of symptoms, there is debate about whether the diagnosis represents a single disorder or a number of discrete syndromes. For this reason, Eugen Bleuler termed the disease the schizophrenias (plural) when he coined the name. Despite its etymology, schizophrenia is not the same as dissociative identity disorder, previously known as multiple personality disorder or split personality, with which it has been erroneously confused.
Increased dopamine activity in the mesolimbic pathway of the brain is consistently found in schizophrenic individuals. The mainstay of treatment is antipsychotic medication; this type of drug primarily works by suppressing dopamine activity. Dosages of antipsychotics are generally lower than in the early decades of their use. Psychotherapy, and vocational and social rehabilitation are also important. In more serious cases - where there is risk to self and others - involuntary hospitalization may be necessary, although hospital stays are less frequent and for shorter periods than they were in previous times.
The disorder is thought to mainly affect cognition, but it also usually contributes to chronic problems with behavior and emotion. People with schizophrenia are likely to have additional (comorbid) conditions, including major depression and anxiety disorders; the lifetime occurrence of substance abuse is around 40%. Social problems, such as long-term unemployment, poverty and homelessness, are common. Furthermore, the averagelife expectancy of people with the disorder is 10 to 12 years less than those without, due to increased physical health problems and a higher suicide rate.
 |
Schizophrenia occurs equally in males and females, although typically appears earlier in men - the peak ages of onset are 20–28 years for males and 26–32 years for females. Onset in childhood is much rarer, as is onset in middle- or old age. The lifetime prevalence of schizophrenia - the proportion of individuals expected to experience the disease at any time in their lives - is commonly given at 1%. However, a 2002 systematic review of many studies found a lifetime prevalence of 0.55%. Despite the received wisdom that schizophrenia occurs at similar rates worldwide, its prevalence varies across the world, within countries, and at the local and neighbourhood level. One particularly stable and replicable finding has been the association between living in an urban environment and schizophrenia diagnosis, even after factors such as drug use, ethnic group and size of social group have been controlled for. Schizophrenia is known to be a major cause of disability. In a 1999 study of 14 countries, active psychosis was ranked the third-most-disabling condition after quadriplegia and dementia and ahead ofparaplegia and blindness.
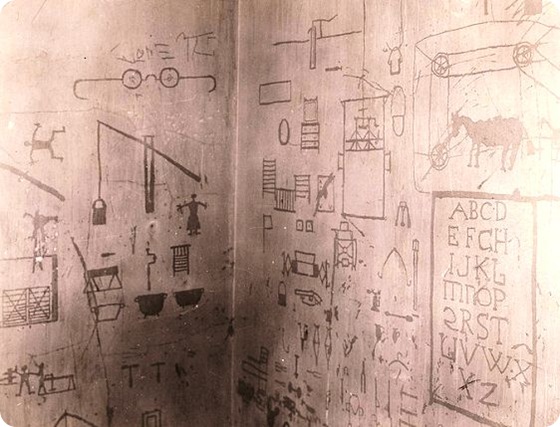
Accounts of a schizophrenia-like syndrome are thought to be rare in the historical record prior to the 1800s, although reports of irrational, unintelligible, or uncontrolled behavior were common. There has been an interpretation that brief notes in the Ancient Egyptian Ebers papyrus may imply schizophrenia, but other reviews have not suggested any connection. A review of ancient Greek and Roman literature indicated that although psychosis was described, there was no account of a condition meeting the criteria for schizophrenia. Bizarre psychotic beliefs and behaviors similar to some of the symptoms of schizophrenia were reported in Arabic medical and psychological literature during the Middle Ages. In The Canon of Medicine, for example, Avicenna described a condition somewhat resembling the symptoms of schizophrenia which he called Junun Mufrit (severe madness), which he distinguished from other forms of madness (Junun) such as mania, rabies and manic depressive psychosis. However, no condition resembling schizophrenia was reported in Şerafeddin Sabuncuoğlu's Imperial Surgery, a major Islamic medical textbook of the 15th century. Given limited historical evidence, schizophrenia (as prevalent as it is today) may be a modern phenomenon, or alternatively it may have been obscured in historical writings by related concepts such as melancholia or mania.
A detailed case report in 1797 concerning James Tilly Matthews, and accounts by Phillipe Pinel published in 1809, are often regarded as the earliest cases of schizophrenia in the medical and psychiatric literature. Schizophrenia was first described as a distinct syndrome affecting teenagers and young adults by Bénédict Morel in 1853, termed démence précoce (literally 'early dementia'). The term dementia praecox was used in 1891 by Arnold Pick to in a case report of a psychotic disorder. In 1893 Emil Kraepelin introduced a broad new distinction in the classification of mental disorders between dementia praecox and mood disorder (termed manic depression and including both unipolar and bipolar depression). Kraepelin believed that dementia praecox was primarily a disease of the brain, and particularly a form of dementia, distinguished from other forms of dementia, such as Alzheimer's disease, which typically occur later in life. Kraepelin's classification slowly gained acceptance. There were objections to the use of the term "dementia" despite cases of recovery, and some defence of diagnoses it replaced such as adolescent insanity.
The word schizophrenia - which translates roughly as "splitting of the mind" and comes from the Greek roots schizein (σχίζειν, "to split") and phrēn, phren- (φρήν, φρεν-, "mind") - was coined by Eugen Bleuler in 1908 and was intended to describe the separation of function between personality, thinking, memory, and perception. Bleuler described the main symptoms as 4 A's: flattened Affect, Autism, impaired Association of ideas and Ambivalence. Bleuler realized that the illness was not a dementia as some of his patients improved rather than deteriorated and hence proposed the term schizophrenia instead.
The term schizophrenia is commonly misunderstood to mean that affected persons have a "split personality". Although some people diagnosed with schizophrenia may hear voices and may experience the voices as distinct personalities, schizophrenia does not involve a person changing among distinct multiple personalities. The confusion arises in part due to the meaning of Bleuler's term schizophrenia (literally "split" or "shattered mind"). The first known misuse of the term to mean "split personality" was in an article by the poet T. S. Eliot in 1933.
In the first half of the twentieth century schizophrenia was considered to be a hereditary defect, and sufferers were subject to eugenics in many countries. Hundreds of thousands were sterilized, with or without consent - the majority in Nazi Germany, the United States, and Scandinavian countries. Along with other people labeled "mentally unfit", many diagnosed with schizophrenia were murdered in the Nazi "Action T4" program.
In the early 1970s, the diagnostic criteria for schizophrenia was the subject of a number of controversies which eventually led to the operational criteria used today. It became clear after the 1971 US-UK Diagnostic Study that schizophrenia was diagnosed to a far greater extent in America than in Europe. This was partly due to looser diagnostic criteria in the US, which used the DSM-II manual, contrasting with Europe and its ICD-9. David Rosenhan's 1972 study, published in the journal Science under the title On being sane in insane places, concluded that the diagnosis of schizophrenia in the US was often subjective and unreliable. These were some of the factors in leading to the revision not only of the diagnosis of schizophrenia, but the revision of the whole DSM manual, resulting in the publication of the DSM-III in 1980. Since the 1970s more than 40 diagnostic criteria for schizophrenia have been proposed and evaluated.
In the Soviet Union the diagnosis of schizophrenia has also been used for political purposes. The prominent Soviet psychiatrist Andrei Snezhnevsky created and promoted an additional sub-classification of sluggishly progressing schizophrenia. This diagnosis was used to discredit and expeditiously imprison political dissidents while dispensing with a potentially embarrassing trial. The practice was exposed to Westerners by a number of Soviet dissidents, and in 1977 the World Psychiatric Association condemned the Soviet practice at the Sixth World Congress of Psychiatry. Rather than defending his theory that a latent form of schizophrenia caused dissidents to oppose the regime, Snezhnevsky broke all contact with the West in 1980 by resigning his honorary positions abroad.
Social stigma has been identified as a major obstacle in the recovery of patients with schizophrenia. In a large, representative sample from a 1999 study, 12.8% of Americans believed that individuals with schizophrenia were "very likely" to do something violent against others, and 48.1% said that they were "somewhat likely" to. Over 74% said that people with schizophrenia were either "not very able" or "not able at all" to make decisions concerning their treatment, and 70.2% said the same of money management decisions. The perception of individuals with psychosis as violent has more than doubled in prevalence since the 1950s, according to one meta-analysis.
Schizophrenia Causes
The causes of schizophrenia have been the subject of much debate, with various factors proposed and discounted. Studies suggest that genetics, prenatal development, early environment, neurobiology and psychological and social processes are important contributory factors. Current psychiatric research into the development of the disorder is often based on a neurodevelopmental model. In the absence of a confirmed specificpathology underlying the diagnosis, some question the legitimacy of schizophrenia's status as a disease. Furthermore, some propose that the perceptions and feelings involved are meaningful and do not necessarily involve impairment.
Although no common cause of schizophrenia has been identified in all individuals diagnosed with the condition, currently most researchers and clinicians believe it results from a combination of both brain vulnerabilities (either inherited or acquired) and life events. This widely-adopted approach is known as the 'stress-vulnerability' model, and much scientific debate now focuses on how much each of these factors contributes to the development and maintenance of schizophrenia. Schizophrenia is most commonly first diagnosed during late adolescence or early adulthood, suggesting it is often the end process of childhood and adolescent development. There is on average a somewhat earlier onset for men than women, with the possible influence of the female hormoneestrogen being one hypothesis and sociocultural influences another.
After reviewing techniques like: Genome Wide Association Studies; Single Neucleotide Polymorphisms and Copy Number Variations; the Nature journal reports: the basic observation is that, "You have this clear tangible phenomenon in which children resemble their parents"...."Despite what children get told in elementary school science we just don't know how that works," as Professor of ecology and evolutionary biology at Princeton, Leonid Kruglyak says (in reviewing hereditibility in general); . It cites schizophrenia as a trait in which the genes have gone missing.
Both individual twin studies and meta-analyses of twin studies estimate the heritability of risk for schizophrenia to be approximately 80% (this refers to the proportion of variation between individuals in a population that is influenced by genetic factors, not the degree of genetic determination of individual risk). Adoption studies have also indicated a somewhat increased risk in those with a parent with schizophrenia even when raised apart. Studies suggest that the phenotype is genetically influenced but not genetically determined; that the variants in genes are generally within the range of normal human variation and have low risk associated with them each individually; and that some interact with each other and with environmental risk factors; and that they may not be specific to schizophrenia. Some twin studies have found rates as low as 11.0%–13.8% among monozygotic twins, and 1.8%–4.1% among dizygotic twins, however. In the "Pairs of Veteran Twins" study, for example, 338 pairs were schizophrenic with only 26 pairs concordant, and it was concluded in one report: "the role of the suggested genetic factor appears to be a limited one; 85 percent of the affected monozygotic pairs in the sample were discordant for schizophrenia". In addition, some scientists criticize the methodology of the twin studies, and have argued that the genetic basis of schizophrenia is still largely unknown or open to different interpretations.
A great deal of effort has been put into molecular genetic studies of schizophrenia, which attempt to identify specific genes which may increase risk. A 2003 review of linkage studies listed seven genes as likely to increase risk for a later diagnosis of the disorder. Two recent reviews suggested that the evidence was strongest for two genesknown as dysbindin (DTNBP1) and neuregulin (NRG1), and that a number of other genes (such as COMT, RGS4, PPP3CC, ZDHHC8, DISC1, and AKT1) showed some early promising results. Variations near the gene FXYD6 have also been associated with schizophrenia in the UK but not in Japan. In 2008, rs7341475 SNP of the reelin gene was associated with an increased risk of schizophrenia in women, but not in men. This female-specific association was replicated in several populations.
The largest most comprehensive genetic study of its kind, involving tests of several hundred single nucleotide polymorphisms (SNPs) in nearly 1,900 individuals with schizophrenia or schizoaffective disorder and 2,000 comparison subjects, reported in 2008 that there was no evidence of any significant association between the disorders and any of 14 previously identified candidate genes (RGS4, DISC1, DTNBP1, STX7,TAAR6, PPP3CC, NRG1, DRD2, HTR2A, DAOA, AKT1, CHRNA7, COMT, and ARVCF). The statistical distributions suggested nothing more than chance variation. The authors concluded that the findings make it unlikely that common SNPs in these genes account for a substantial proportion of the genetic risk for schizophrenia, although small effects could not be ruled out.
The perhaps largest analysis of genetic associations in schizophrenia is with the SzGenedatabase at the Schizophrenia Research Forum. One 2008 meta-analysis examined genetic variants in 16 genes and found nominally significant effects.
Other research has suggested that a greater than average number of rare deletions or duplications of tiny DNA sequences within genes (known as copy number variants) are linked to increased risk for schizophrenia, especially in those "sporadic" cases not linked to family history of schizophrenia, and that the genetic factors and developmental pathways can thus be different in different individuals. A genome wide survey of 3,391 individuals with schizophrenia found CNVs in less than 1% of cases. Within them, deletions in regions related to psychosis were observed, as well as deletions onchromosome 15q13.3 and 1q21.1. CNVs occur due to non-homologous allelic recombination mediated by low copy repeats (sequentially similar regions). This results in deletions and duplications of dosage sensitive genes. It has been speculated that CNVs underlie a significant proportion of normal human variation, including differences in cognitive, behavioral, and psychological features, and that CNVs in at least three loci can result in increased risk for schizophrenia in a few individuals.. Epigenetics may also play a role in schizophrenia, with the expression of Protocadherin 11 X/Y playing a possible role in schizophrenia.
A 2009 study was able to create mice matching schizophrenic symptoms by the deletion of only one gene set, those of the neuregulin post-synaptic receptor. The result showed that although the mice mostly developed normally, on further brain development, glutamate receptors brokedown. This theory supports the glutamate hypothesis of schizophrenia.
One epidemiological finding is that people diagnosed with schizophrenia are more likely to have been born in winter or spring (at least in the northern hemisphere). However, the effect is not large. Explanations have included a greater prevalence of viral infections at that time, or a greater likelihood of vitamin D deficiency. A similar effect (increased likelihood of being born in winter and spring) has also been found with other, healthy populations, such as chess players. Women who were pregnant during the Dutch famine of 1944, where many people were close to starvation (experiencing malnutrition) had a higher chance of having a child who would later develop schizophrenia. Studies of Finnish mothers who were pregnant when they found out that their husbands had been killed during the Winter War of 1939–1940 have shown that their children were significantly more likely to develop schizophrenia when compared with mothers who found out about their husbands' death after pregnancy, suggesting that maternal stress may have an effect.
Animal models have suggested links between intrauterine growth restriction and specific neurological abnormalities similar to those that may be involved in the development ofschizophrenia, including ventricular enlargement and reduced hippocampal volume in guinea pigs.
A longitudinal study found that obstetric complications involving hypoxia were one factor associated with neurodevelopmental impairments in childhood and with the later development of schizophreniform disorders. Fetal hypoxia has been found to predict unusual movements at age 4 (but not age 7) among children who go on to develop schizophrenia, suggesting that its effects are specific to the stage of neurodevelopment. A Japanese case study of monozygotic twins discordant forschizophrenia (one has the diagnosis while the other does not) draws attention to their different weights at birth and concludes hypoxia may be the differentiating factor. The unusual functional laterality in speech production (e.g. right hemisphere auditory processing) found in some individuals with schizophrenia could be due to aberrant neural networks established as a compensation for left temporal lobe damage induced by pre- or perinatal hypoxia. Prenatal and perinatal hypoxia appears to be important as one factor in the neurodevelopmental model, with the important implication that some forms of schizophrenia may thus be preventable.
Research on rodents seeking to understand the possible role of prenatal hypoxia in disorders such as schizophrenia has indicated that it can lead to a range of sensorimotor and learning/memory abnormalities. Impairments in motor function and coordination, evident on challenging tasks when the hypoxia was severe enough to cause brain damage, were long-lasting and described as a "hallmark of prenatal hypoxia". Several animal studies have indicated that fetal hypoxia can affect many of the same neural substrates implicated in schizophrenia, depending on the severity and duration of the hypoxic event as well as the period of gestation, and in humans moderate or severe (but not mild) fetal hypoxia has been linked to a series of motor, language and cognitive deficits in children, regardless of genetic liability toschizophrenia.
Whereas most studies find only a modest effect of hypoxia in schizophrenia, a longitudinal study using a combination of indicators to detect possible fetal hypoxia, such as early equivalents of Neurological Soft Signs or obstetric complications, reported that the risk of schizophrenia and other nonaffective psychoses was "strikingly elevated" (5.75% versus 0.39%).
Influenza has long been studied as a possible factor. A 1988 study found that individuals who were exposed to the Asian flu as second trimester fetuses were at increased risk of eventually developing schizophrenia. This result was corroborated by a later British study of the same pandemic,, but not by a 1994 study of the pandemic in Croatia. A Japanese study also found no support for a link between schizophrenia and birth after an influenza epidemic.
Polio, measles, varicella-zoster, rubella, herpes simplex virus type 2, maternal genital infections, and more recently Toxoplasma gondii, have been correlated with the later development of schizophrenia. Psychiatrists E. Fuller Torrey and R.H. Yolken have hypothesized that the latter, a common parasite in humans, contributes to some, if not many, cases of schizophrenia. In a meta-analysis of several studies, they found moderately higher levels of Toxoplasma antibodies in those with schizophrenia and possibly higher rates of prenatal or early postnatal exposure to Toxoplasma gondii, but not acute infection. However, in another study of postmortem brain tissue, the authors have reported equivocal or negative results, including no evidence of herpes virus or T. gondii involvement in schizophrenia.
There is some evidence for the role of autoimmunity in the development of some cases of schizophrenia. A statistical correlation has been reported with various autoimmune diseases and direct studies have linked dysfunctional immune status to some of the clinical features of schizophrenia.
A prospective study found average differences across a range of developmental domains, including reaching milestones of motor development at a later age, having more speech problems, lower educational test results, solitary play preferences at ages four and six, and being more socially anxious at age 13. Lower ratings of the mother's skills and understanding of the child at age 4 were also related.
Some of the early developmental differences were identified in the first year of life in a study in Finland, although generally related to psychotic disorders rather than schizophrenia in particular. The early subtle motor signs persisted to some extent, showing a small link to later school performance in adolescence. An earlier Finnish study found that childhood performance of 400 individuals diagnosed with schizophrenia was significantly worse than controls on subjects involving motor co-ordination (sports and handcrafts) between ages 7 and 9, but there were no differences on academic subjects (contrary to some other IQ findings). (Patients in this age group with these symptoms were significantly less likely to progress to high school, despite academic ability) However, reanalysis of the data from the later Finnish study, on older children (14 to 16) in a changed school system, using narrower diagnostic criteria and with less cases but more controls, did not support a significant difference on sports and handicraft performance. However, another study found that unusual motor coordination scores at 7 years of age were associated in adulthood with both those with schizophrenia and their unaffected siblings, while unusual movements at ages 4 and 7 predicted adultschizophrenia but not unaffected sibling status.
A birth cohort study in New Zealand found that children who went on to develop schizophreniform disorder had, as well as emotional problems and interpersonal difficulties linked to all adult psychiatric outcomes measured, significant impairments in neuromotor, receptive language, and cognitive development. A retrospective study found that adults with schizophrenia had performed better than average in artistic subjects at ages 12 and 15, and in linguistic and religious subjects at age 12, but worse than average in gymnastics at age 15.
Some small studies on offspring of individuals with schizophrenia have identified various neurobehavioral deficits, a poorer family environment and disruptive school behaviour, poor peer engagement, immaturity or unpopularity or poorer social competence and increasing schizophrenic symptomology emerging during adolescence.
A minority "deficit syndrome" subtype of schizophrenia is proposed to be more marked by early poor adjustment and behavioral problems, as compared to non-deficit subtypes.
The rate of substance use is known to be particularly high in this group. In a recent study, 60% of people with schizophrenia were found to use substances and 37% would be diagnosable with a substance use disorder.
Drugs such as ketamine, PCP, and LSD have been used to mimic schizophrenia for research purposes. Using LSD and other psychedelics as a model has now fallen out of favor with the scientific research community, as the differences between the drug induced states and the typical presentation of schizophrenia have become clear. The dissociatives ketamine and PCP are still considered to produce states that are remarkably similar however.
An older longitudinal study, published in 1987, suggested sixfold increase of schizophrenia risks for high consumers of cannabis (use on more than fifty occasions) in Sweden.
Despite increases in cannabis consumption in the 1960s and 1970s in western society, rates of psychotic disorders such as schizophrenia remained relatively stable. Sweden and Japan, where self-reported marijuana use is very low, do not have lower rates of psychosis than the U.S. and Canada do. For the theory of true causality to be correct, other factors which are thought to contribute to schizophrenia would have to have converged almost flawlessly to mask the effect of increased cannabis usage.
Despite the higher prevalence of tobacco smoking, people diagnosed with schizophreniahave a much lower than average chance of developing and dying from lung cancer. While the reason for this is unknown, it may be because of a genetic resistance to thecancer, a side-effect of drugs being taken, or a statistical effect of increased likelihood of dying from causes other than lung cancer.
A 2003 study of over 50,000 Swedish conscripts found that there was a small but significant protective effect of smoking cigarettes on the risk of developing schizophrenia later in life. While the authors of the study stressed that the risks of smoking far outweigh these minor benefits, this study provides further evidence for the 'self-medication' theory of smoking in schizophrenia and may give clues as to how schizophrenia might develop at the molecular level. Furthermore, many people with schizophrenia have smoked tobacco products long before they are diagnosed with the illness, and some groups advocate that the chemicals in tobacco have actually contributed to the onset of the illness and have no benefit of any kind.
It is of interest that cigarette smoking affects liver function such that the antipsychotic drugs used to treat schizophrenia are broken down in the blood stream more quickly. This means that smokers with schizophrenia need slightly higher doses of antipsychotic drugs in order for them to be effective than do their non-smoking counterparts.
The increased rate of smoking in schizophrenia may be due to a desire to self-medicate with nicotine. One possible reason is that smoking produces a short term effect to improve alertness and cognitive functioning in persons who suffer this illness. It has been postulated that the mechanism of this effect is that people with schizophrenia have a disturbance of nicotinic receptor functioning which is temporarily abated by tobacco use.
A study from 1989 and a 2004 case study show that when haloperidol is administered, nicotine limits the extent to which the antipsychotic increases the sensitivity of the dopamine 2 receptor. Dependent on the dopamine system, symptoms of Tardive Dyskinesia are not found in the nicotine administered patients despite a roughly 70% increase in dopamine receptor activity, but the controls have more than 90% and do develop symptoms.A 1997 study showed that akathisia was significantly reduced upon administration of nicotine when the akathisia was induced by antipsychotics. This gives credence to the idea tobacco could be used to self medicate by limiting effects of the illness, the medication, or both.
Although no common cause of schizophrenia has been identified in all individuals diagnosed with the condition, currently most researchers and clinicians believe it results from a combination of both brain vulnerabilities (either inherited or acquired) and life events. This widely-adopted approach is known as the 'stress-vulnerability' model, and much scientific debate now focuses on how much each of these factors contributes to the development and maintenance of schizophrenia. Schizophrenia is most commonly first diagnosed during late adolescence or early adulthood, suggesting it is often the end process of childhood and adolescent development. There is on average a somewhat earlier onset for men than women, with the possible influence of the female hormoneestrogen being one hypothesis and sociocultural influences another.
Genetics
Evidence suggests that genetic vulnerability and environmental factors can act in combination to result in diagnosis of schizophrenia. Research suggests that genetic vulnerability to schizophrenia is multifactorial, caused by interactions of several genes.After reviewing techniques like: Genome Wide Association Studies; Single Neucleotide Polymorphisms and Copy Number Variations; the Nature journal reports: the basic observation is that, "You have this clear tangible phenomenon in which children resemble their parents"...."Despite what children get told in elementary school science we just don't know how that works," as Professor of ecology and evolutionary biology at Princeton, Leonid Kruglyak says (in reviewing hereditibility in general); . It cites schizophrenia as a trait in which the genes have gone missing.
Both individual twin studies and meta-analyses of twin studies estimate the heritability of risk for schizophrenia to be approximately 80% (this refers to the proportion of variation between individuals in a population that is influenced by genetic factors, not the degree of genetic determination of individual risk). Adoption studies have also indicated a somewhat increased risk in those with a parent with schizophrenia even when raised apart. Studies suggest that the phenotype is genetically influenced but not genetically determined; that the variants in genes are generally within the range of normal human variation and have low risk associated with them each individually; and that some interact with each other and with environmental risk factors; and that they may not be specific to schizophrenia. Some twin studies have found rates as low as 11.0%–13.8% among monozygotic twins, and 1.8%–4.1% among dizygotic twins, however. In the "Pairs of Veteran Twins" study, for example, 338 pairs were schizophrenic with only 26 pairs concordant, and it was concluded in one report: "the role of the suggested genetic factor appears to be a limited one; 85 percent of the affected monozygotic pairs in the sample were discordant for schizophrenia". In addition, some scientists criticize the methodology of the twin studies, and have argued that the genetic basis of schizophrenia is still largely unknown or open to different interpretations.
A great deal of effort has been put into molecular genetic studies of schizophrenia, which attempt to identify specific genes which may increase risk. A 2003 review of linkage studies listed seven genes as likely to increase risk for a later diagnosis of the disorder. Two recent reviews suggested that the evidence was strongest for two genesknown as dysbindin (DTNBP1) and neuregulin (NRG1), and that a number of other genes (such as COMT, RGS4, PPP3CC, ZDHHC8, DISC1, and AKT1) showed some early promising results. Variations near the gene FXYD6 have also been associated with schizophrenia in the UK but not in Japan. In 2008, rs7341475 SNP of the reelin gene was associated with an increased risk of schizophrenia in women, but not in men. This female-specific association was replicated in several populations.
The largest most comprehensive genetic study of its kind, involving tests of several hundred single nucleotide polymorphisms (SNPs) in nearly 1,900 individuals with schizophrenia or schizoaffective disorder and 2,000 comparison subjects, reported in 2008 that there was no evidence of any significant association between the disorders and any of 14 previously identified candidate genes (RGS4, DISC1, DTNBP1, STX7,TAAR6, PPP3CC, NRG1, DRD2, HTR2A, DAOA, AKT1, CHRNA7, COMT, and ARVCF). The statistical distributions suggested nothing more than chance variation. The authors concluded that the findings make it unlikely that common SNPs in these genes account for a substantial proportion of the genetic risk for schizophrenia, although small effects could not be ruled out.
The perhaps largest analysis of genetic associations in schizophrenia is with the SzGenedatabase at the Schizophrenia Research Forum. One 2008 meta-analysis examined genetic variants in 16 genes and found nominally significant effects.
Other research has suggested that a greater than average number of rare deletions or duplications of tiny DNA sequences within genes (known as copy number variants) are linked to increased risk for schizophrenia, especially in those "sporadic" cases not linked to family history of schizophrenia, and that the genetic factors and developmental pathways can thus be different in different individuals. A genome wide survey of 3,391 individuals with schizophrenia found CNVs in less than 1% of cases. Within them, deletions in regions related to psychosis were observed, as well as deletions onchromosome 15q13.3 and 1q21.1. CNVs occur due to non-homologous allelic recombination mediated by low copy repeats (sequentially similar regions). This results in deletions and duplications of dosage sensitive genes. It has been speculated that CNVs underlie a significant proportion of normal human variation, including differences in cognitive, behavioral, and psychological features, and that CNVs in at least three loci can result in increased risk for schizophrenia in a few individuals.. Epigenetics may also play a role in schizophrenia, with the expression of Protocadherin 11 X/Y playing a possible role in schizophrenia.
A 2009 study was able to create mice matching schizophrenic symptoms by the deletion of only one gene set, those of the neuregulin post-synaptic receptor. The result showed that although the mice mostly developed normally, on further brain development, glutamate receptors brokedown. This theory supports the glutamate hypothesis of schizophrenia.
Obstetric Events
It is well established that obstetric complications or events are associated with an increased chance of the child later developing schizophrenia, although overall they constitute a non-specific risk factor with a relatively small effect. Obstetric complications occur in approximately 25 to 30% of the general population and the vast majority do not develop schizophrenia, and likewise the majority of individuals with schizophrenia have not had a detectable obstetric event. Nevertheless, the increased average risk is well-replicated, and such events may moderate the effects of genetic or other environmental risk factors. The specific complications or events most linked toschizophrenia, and the mechanisms of their effects, are still under examination.One epidemiological finding is that people diagnosed with schizophrenia are more likely to have been born in winter or spring (at least in the northern hemisphere). However, the effect is not large. Explanations have included a greater prevalence of viral infections at that time, or a greater likelihood of vitamin D deficiency. A similar effect (increased likelihood of being born in winter and spring) has also been found with other, healthy populations, such as chess players. Women who were pregnant during the Dutch famine of 1944, where many people were close to starvation (experiencing malnutrition) had a higher chance of having a child who would later develop schizophrenia. Studies of Finnish mothers who were pregnant when they found out that their husbands had been killed during the Winter War of 1939–1940 have shown that their children were significantly more likely to develop schizophrenia when compared with mothers who found out about their husbands' death after pregnancy, suggesting that maternal stress may have an effect.
Fetal Growth
Lower than average birth weight has been one of the most consistent findings, indicating slowed fetal growth possibly mediated by genetic effects. Almost any factor adversely affecting the fetus will affect growth rate, however, so the association has been described as not particularly informative regarding causation. In addition, the majority of birth cohort studies have failed to find a link between schizophrenia and low birth weight or other signs of growth retardation.Animal models have suggested links between intrauterine growth restriction and specific neurological abnormalities similar to those that may be involved in the development ofschizophrenia, including ventricular enlargement and reduced hippocampal volume in guinea pigs.
Hypoxia
It has been hypothesized since the 1970s that brain hypoxia (low oxygen levels) before, at or immediately after birth may be a risk factor for the development of schizophrenia. This has been recently described as one of the most important of the external factors that influence susceptibility, although studies have been mainly epidemiological. Fetal hypoxia, in the presence of certain unidentified genes, has been correlated with reduced volume of the hippocampus, which is in turn correlated with schizophrenia. Although most studies have interpreted hypoxia as causing some form of neuronal dysfunction or even subtle damage, it has been suggested that the physiological hypoxia that prevails in normal embryonic and fetal development, or pathological hypoxia or ischemia, may exert an effect by regulating or dysregulating genes involved in neurodevelopment. A literature review judged that over 50% of the candidate genes for susceptibility to schizophrenia met criteria for "ischemia–hypoxia regulation and/or vascular expression".A longitudinal study found that obstetric complications involving hypoxia were one factor associated with neurodevelopmental impairments in childhood and with the later development of schizophreniform disorders. Fetal hypoxia has been found to predict unusual movements at age 4 (but not age 7) among children who go on to develop schizophrenia, suggesting that its effects are specific to the stage of neurodevelopment. A Japanese case study of monozygotic twins discordant forschizophrenia (one has the diagnosis while the other does not) draws attention to their different weights at birth and concludes hypoxia may be the differentiating factor. The unusual functional laterality in speech production (e.g. right hemisphere auditory processing) found in some individuals with schizophrenia could be due to aberrant neural networks established as a compensation for left temporal lobe damage induced by pre- or perinatal hypoxia. Prenatal and perinatal hypoxia appears to be important as one factor in the neurodevelopmental model, with the important implication that some forms of schizophrenia may thus be preventable.
Research on rodents seeking to understand the possible role of prenatal hypoxia in disorders such as schizophrenia has indicated that it can lead to a range of sensorimotor and learning/memory abnormalities. Impairments in motor function and coordination, evident on challenging tasks when the hypoxia was severe enough to cause brain damage, were long-lasting and described as a "hallmark of prenatal hypoxia". Several animal studies have indicated that fetal hypoxia can affect many of the same neural substrates implicated in schizophrenia, depending on the severity and duration of the hypoxic event as well as the period of gestation, and in humans moderate or severe (but not mild) fetal hypoxia has been linked to a series of motor, language and cognitive deficits in children, regardless of genetic liability toschizophrenia.
Whereas most studies find only a modest effect of hypoxia in schizophrenia, a longitudinal study using a combination of indicators to detect possible fetal hypoxia, such as early equivalents of Neurological Soft Signs or obstetric complications, reported that the risk of schizophrenia and other nonaffective psychoses was "strikingly elevated" (5.75% versus 0.39%).
Other factors
There is an emerging literature on a wide range of prenatal risk factors, such as prenatal stress, intrauterine (in the womb) malnutrition, and prenatal infection. Increased parental age has been linked, possibly due to prenatal complications increasing the risk of genetic mutations. Maternal-fetal rhesus or genotype incompatibility has also been linked, via increasing the risk of an adverse prenatal environment. And, in mothers with schizophrenia, an increased risk has been identified via a complex interaction between maternal genotype, maternal behavior, prenatal environment and possibly medication and socioeconomic factors.Infections
Numerous viral infections, in utero or in childhood, have been associated with an increased risk of later developing schizophrenia. Schizophrenia is somewhat more common in those born in winter to early spring, when infections are more common.Influenza has long been studied as a possible factor. A 1988 study found that individuals who were exposed to the Asian flu as second trimester fetuses were at increased risk of eventually developing schizophrenia. This result was corroborated by a later British study of the same pandemic,, but not by a 1994 study of the pandemic in Croatia. A Japanese study also found no support for a link between schizophrenia and birth after an influenza epidemic.
Polio, measles, varicella-zoster, rubella, herpes simplex virus type 2, maternal genital infections, and more recently Toxoplasma gondii, have been correlated with the later development of schizophrenia. Psychiatrists E. Fuller Torrey and R.H. Yolken have hypothesized that the latter, a common parasite in humans, contributes to some, if not many, cases of schizophrenia. In a meta-analysis of several studies, they found moderately higher levels of Toxoplasma antibodies in those with schizophrenia and possibly higher rates of prenatal or early postnatal exposure to Toxoplasma gondii, but not acute infection. However, in another study of postmortem brain tissue, the authors have reported equivocal or negative results, including no evidence of herpes virus or T. gondii involvement in schizophrenia.
There is some evidence for the role of autoimmunity in the development of some cases of schizophrenia. A statistical correlation has been reported with various autoimmune diseases and direct studies have linked dysfunctional immune status to some of the clinical features of schizophrenia.
Childhood Antecedents
In general, the antecedents of schizophrenia are subtle and those who will go on to develop schizophrenia do not form a readily identifiable subgroup. Average group differences from the norm may be in the direction of superior as well as inferior performance. Overall, birth cohort studies have indicated subtle nonspecific behavioral features, some evidence for psychotic-like experiences (particularly hallucinations), and various cognitive antecedents. There have been some inconsistencies in the particular domains of functioning identified and whether they continue through childhood and whether they are specific to schizophrenia.A prospective study found average differences across a range of developmental domains, including reaching milestones of motor development at a later age, having more speech problems, lower educational test results, solitary play preferences at ages four and six, and being more socially anxious at age 13. Lower ratings of the mother's skills and understanding of the child at age 4 were also related.
Some of the early developmental differences were identified in the first year of life in a study in Finland, although generally related to psychotic disorders rather than schizophrenia in particular. The early subtle motor signs persisted to some extent, showing a small link to later school performance in adolescence. An earlier Finnish study found that childhood performance of 400 individuals diagnosed with schizophrenia was significantly worse than controls on subjects involving motor co-ordination (sports and handcrafts) between ages 7 and 9, but there were no differences on academic subjects (contrary to some other IQ findings). (Patients in this age group with these symptoms were significantly less likely to progress to high school, despite academic ability) However, reanalysis of the data from the later Finnish study, on older children (14 to 16) in a changed school system, using narrower diagnostic criteria and with less cases but more controls, did not support a significant difference on sports and handicraft performance. However, another study found that unusual motor coordination scores at 7 years of age were associated in adulthood with both those with schizophrenia and their unaffected siblings, while unusual movements at ages 4 and 7 predicted adultschizophrenia but not unaffected sibling status.
A birth cohort study in New Zealand found that children who went on to develop schizophreniform disorder had, as well as emotional problems and interpersonal difficulties linked to all adult psychiatric outcomes measured, significant impairments in neuromotor, receptive language, and cognitive development. A retrospective study found that adults with schizophrenia had performed better than average in artistic subjects at ages 12 and 15, and in linguistic and religious subjects at age 12, but worse than average in gymnastics at age 15.
Some small studies on offspring of individuals with schizophrenia have identified various neurobehavioral deficits, a poorer family environment and disruptive school behaviour, poor peer engagement, immaturity or unpopularity or poorer social competence and increasing schizophrenic symptomology emerging during adolescence.
A minority "deficit syndrome" subtype of schizophrenia is proposed to be more marked by early poor adjustment and behavioral problems, as compared to non-deficit subtypes.
Substance Use
The relationship between schizophrenia and drug use is complex, meaning that a clear causal connection between drug use and schizophrenia has been difficult to tease apart. There is strong evidence that using certain drugs can trigger either the onset or relapse of schizophrenia in some people. It may also be the case, however, that people with schizophrenia use drugs to overcome negative feelings associated with both the commonly prescribed antipsychotic medication and the condition itself, where negative emotion, paranoia and anhedonia are all considered to be core features.The rate of substance use is known to be particularly high in this group. In a recent study, 60% of people with schizophrenia were found to use substances and 37% would be diagnosable with a substance use disorder.
Amphetamines
As amphetamines trigger the release of dopamine and excessive dopamine function is believed to be responsible for many symptoms of schizophrenia (known as the dopamine hypothesis of schizophrenia), amphetamines may worsen schizophrenia symptoms.Hallucinogens
Schizophrenia can sometimes be triggered by heavy use of hallucinogenic or stimulant drugs, although some claim that a predisposition towards developing schizophrenia is needed for this to occur. There is also some evidence suggesting that people suffering schizophrenia but responding to treatment can have relapse because of subsequent drug use.Drugs such as ketamine, PCP, and LSD have been used to mimic schizophrenia for research purposes. Using LSD and other psychedelics as a model has now fallen out of favor with the scientific research community, as the differences between the drug induced states and the typical presentation of schizophrenia have become clear. The dissociatives ketamine and PCP are still considered to produce states that are remarkably similar however.
Cannabis
There is some evidence that cannabis use can contribute to schizophrenia. Some studies suggest that cannabis is neither a sufficient nor necessary factor in developing schizophrenia, but that cannabis may significantly increase the risk of developing schizophrenia and may be, among other things, a significant causal factor. Nevertheless, some previous research in this area has been criticised as it has often not been clear whether cannabis use is a cause or effect of schizophrenia. To address this issue, a recent review of studies from which a causal contribution to schizophrenia can be assessed has suggested that cannabis statistically doubles the risk of developing schizophrenia on the individual level, and may, assuming a causal relationship, be responsible for up to 8% of cases in the population.An older longitudinal study, published in 1987, suggested sixfold increase of schizophrenia risks for high consumers of cannabis (use on more than fifty occasions) in Sweden.
Despite increases in cannabis consumption in the 1960s and 1970s in western society, rates of psychotic disorders such as schizophrenia remained relatively stable. Sweden and Japan, where self-reported marijuana use is very low, do not have lower rates of psychosis than the U.S. and Canada do. For the theory of true causality to be correct, other factors which are thought to contribute to schizophrenia would have to have converged almost flawlessly to mask the effect of increased cannabis usage.
Tobacco Use
People with schizophrenia tend to smoke significantly more tobacco than the general population. The rates are exceptionally high amongst institutionalized patients and homeless people. In a UK census from 1993, 74% of people with schizophrenia living in institutions were found to be smokers. A 1999 study that covered all people with schizophrenia in Nithsdale, Scotland found a 58% prevalence rate of cigarette smoking, to compare with 28% in the general population. An older study found that as much as 88% of outpatients with schizophrenia were smokers.Despite the higher prevalence of tobacco smoking, people diagnosed with schizophreniahave a much lower than average chance of developing and dying from lung cancer. While the reason for this is unknown, it may be because of a genetic resistance to thecancer, a side-effect of drugs being taken, or a statistical effect of increased likelihood of dying from causes other than lung cancer.
A 2003 study of over 50,000 Swedish conscripts found that there was a small but significant protective effect of smoking cigarettes on the risk of developing schizophrenia later in life. While the authors of the study stressed that the risks of smoking far outweigh these minor benefits, this study provides further evidence for the 'self-medication' theory of smoking in schizophrenia and may give clues as to how schizophrenia might develop at the molecular level. Furthermore, many people with schizophrenia have smoked tobacco products long before they are diagnosed with the illness, and some groups advocate that the chemicals in tobacco have actually contributed to the onset of the illness and have no benefit of any kind.
It is of interest that cigarette smoking affects liver function such that the antipsychotic drugs used to treat schizophrenia are broken down in the blood stream more quickly. This means that smokers with schizophrenia need slightly higher doses of antipsychotic drugs in order for them to be effective than do their non-smoking counterparts.
The increased rate of smoking in schizophrenia may be due to a desire to self-medicate with nicotine. One possible reason is that smoking produces a short term effect to improve alertness and cognitive functioning in persons who suffer this illness. It has been postulated that the mechanism of this effect is that people with schizophrenia have a disturbance of nicotinic receptor functioning which is temporarily abated by tobacco use.
A study from 1989 and a 2004 case study show that when haloperidol is administered, nicotine limits the extent to which the antipsychotic increases the sensitivity of the dopamine 2 receptor. Dependent on the dopamine system, symptoms of Tardive Dyskinesia are not found in the nicotine administered patients despite a roughly 70% increase in dopamine receptor activity, but the controls have more than 90% and do develop symptoms.A 1997 study showed that akathisia was significantly reduced upon administration of nicotine when the akathisia was induced by antipsychotics. This gives credence to the idea tobacco could be used to self medicate by limiting effects of the illness, the medication, or both.
Life Experiences
The chance of developing schizophrenia has been found to increase with the number of adverse social factors (e.g. indicators of socioeconomic disadvantage or social exclusion) present in childhood. Stressful life events generally precede the onset ofschizophrenia. A personal or recent family history of migration is a considerable risk factor for schizophrenia, which has been linked to psychosocial adversity, social defeat from being an outsider, racial discrimination, family dysfunction, unemployment and poor housing conditions. Childhood experiences of abuse or trauma are risk factors for a diagnosis of schizophrenia later in life. Recent large-scale general population studies indicate the relationship is a causal one, with an increasing risk with additional experiences of maltreatment, although a critical review suggests conceptual and methodological issues require further research. There is some evidence that adversities may lead to cognitive biases and/or altered dopamine neurotransmission, a process that has been termed "sensitization". Specific social experiences have been linked to specific psychological mechanisms and psychotic experiences in schizophrenia. In addition, structural neuroimaging studies of victims of sexual abuse and other traumas have sometimes reported findings similar to those sometimes found in psychotic patients, such as thinning of the corpus callosum, loss of volume in the anterior cingulate cortex, and reduced hippocampal volume.Urbanicity
A particularly stable and replicable finding has been the association between living in an urban environment and the development of schizophrenia, even after factors such as drug use, ethnic group and size of social group have been controlled for. A recent study of 4.4 million men and women in Sweden found an 68%–77% increased risk of diagnosed psychosis for people living in the most urbanized environments, a significant proportion of which is likely to be described as schizophrenia. The effect does not appear to be due to a higher incidence of obstetric complications in urban environments. The risk increases with the number of years and degree of urban living in childhood and adolescence, suggesting that constant, cumulative, or repeated exposures during upbringing occurring more frequently in urbanized areas are responsible for the association. Various possible explanations for the effect have been judged unlikely based on the nature of the findings, including infectious causes or a generic stress effect. It is thought to interact with genetic dispositions and, since there appears to be nonrandom variation even across different neighborhoods, and an independent association with social isolation, it has been proposed that the degree of "social capital" (e.g. degree of mutual trust, bonding and safety in neighborhoods) can exert a developmental impact on children growing up in these environments.Close Relationships
Evidence is consistent that negative attitudes from others increase the risk of schizophrenia relapse, in particular critical comments, hostility, authoritarian, and intrusive or controlling attitudes (termed 'high expressed emotion' by researchers). Although family members and significant others are not held responsible for schizophrenia - the attitudes, behaviors and interactions of all parties are addressed - unsupportive dysfunctional relationships may also contribute to an increased risk of developing schizophrenia.Schizophrenia Diagnosis
Schizophrenia is diagnosed on the basis of symptom profiles. Neural correlates do not provide sufficiently useful criteria. Diagnosis is based on the self-reported experiences of the person, and abnormalities in behavior reported by family members, friends or co-workers, followed by a clinical assessment by a psychiatrist, social worker, clinical psychologist or other mental health professional. Psychiatric assessment includes a psychiatric history and some form of mental status examination.
According to the revised fourth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV-TR), to be diagnosed with schizophrenia, three diagnostic criteria must be met:
A more general medical and neurological examination may be needed to rule out medical illnesses which may rarely produce psychotic schizophrenia-like symptoms, such as metabolic disturbance, systemic infection, syphilis, HIV infection, epilepsy, and brainlesions. It may be necessary to rule out a delirium, which can be distinguished by visual hallucinations, acute onset and fluctuating level of consciousness, and indicates an underlying medical illness. Investigations are not generally repeated for relapse unless there is a specific medical indication or possible adverse effects from antipsychotic medication.
"Schizophrenia" does not mean dual personality, despite the etymology of the word (Greek σχίζω = "I split").
The discrete category of schizophrenia used in the DSM has also been criticized. As with other psychiatric disorders, some psychiatrists have suggested that the diagnosis would be better addressed as individual dimensions along which everyone varies, such that there is a spectrum or continuum rather than a cut-off between normal and ill. This approach appears consistent with research on schizotypy, and with a relatively high prevalence of psychotic experiences, mostly non-distressing delusional beliefs, among the general public. In concordance with this observation, psychologist Edgar Jones, and psychiatrists Tony David and Nassir Ghaemi, surveying the existing literature on delusions, pointed out that the consistency and completeness of the definition ofdelusion have been found wanting by many; delusions are neither necessarily fixed, nor false, nor involve the presence of incontrovertible evidence.
Nancy Andreasen, a leading figure in schizophrenia research, has criticized the current DSM-IV and ICD-10 criteria for sacrificing validity for the sake of improving diagnostic reliability. She argues that overemphasis on psychosis in the diagnostic criteria, while improving diagnostic reliability, ignores more fundamental cognitive impairments that are harder to assess due to large variations in presentation. This view is supported by other psychiatrists. In the same vein, Ming Tsuang and colleagues argue that psychotic symptoms may be a common end-state in a variety of disorders, including schizophrenia, rather than a reflection of the specific etiology of schizophrenia, and warn that there is little basis for regarding DSM’s operational definition as the "true" construct of schizophrenia. Neuropsychologist Michael Foster Green went further in suggesting the presence of specific neurocognitive deficits may be used to construct phenotypes that are alternatives to those that are purely symptom-based. These deficits take the form of a reduction or impairment in basic psychological functions such as memory, attention, executive function and problem solving.
The exclusion of affective components from the criteria for schizophrenia, despite their ubiquity in clinical settings, has also become a bone of contention. This exclusion in the DSM has resulted in a "rather convoluted" separate disorder - schizoaffective disorder. Citing poor interrater reliability, some psychiatrists have totally contested the concept of schizoaffective disorder as a separate entity. The categorical distinction between mood disorders and schizophrenia, known as the Kraepelinian dichotomy, has also been challenged by data from genetic epidemiology.
Most schizophrenia studies have found average reduced volume of the left medial temporal lobe and left superior temporal gyrus, and half of studies have revealed deficits in certain areas of the frontal gyrus, parahippocampal gyrus and temporal gyrus. However, at variance with some findings in individuals with chronic schizophrenia (where use of antipsychotics and other factors may have a confounding effect), significant group differences of temporal lobe and amygdala volumes are not shown in first-episode patients on average. The neurobiological abnormalities are so varied that no single abnormality is observed across the entire group of people with DSM-IV–defined schizophrenia. In addition, it remains unclear whether the structural differences are unique to schizophrenia or cut across the traditional diagnostic boundaries between schizophrenia and affective disorders - though perhaps being unique to conditions withpsychotic features.
Studies of the rare childhood-onset schizophrenia (before age 13) indicate a greater-than-normal loss of grey matter over several years, progressing from the back of the brain to the front, levelling out in early adulthood. Such a pattern of "pruning" occurs as part of normal brain development but appears to be exaggerated in childhood-onset psychotic diagnoses, particularly schizophrenia. Abnormalities in the volume of the ventricles or frontal lobes have also been found in several studies but not in others. Volume changes are most likely glial and vascular rather than purely neuronal, and reduction in grey matter may primarily reflect a reduction of neuropil rather than a deficit in the total number of neurons. Other studies, especially some computational studies, have shown that a reduction in the number of neurons can cause psychotic symptoms. Studies to date have been based on small numbers of the most severe and treatment-resistant patients taking antipsychotics.
Electroencephalograph (EEG) recordings of persons with schizophrenia performing perception oriented tasks showed an absence of gamma band activity in the brain, indicating weak integration of critical neural networks in the brain. Those who experienced intense hallucinations, delusions and disorganized thinking showed the lowest frequency synchronization. None of the drugs taken by the persons scanned had moved neural synchrony back into the gamma frequency range. Gamma band and working memory alterations may be related to alterations in interneurons that produce the neurotransmitter GABA.
Atypical connectivity in the default network and other resting-state networks in the brain has been observed in schizophrenic patients. The greater connectivity in the default network and the task-positive network may reflect excessive orientation of attention to introspection and to extrospection, respectively, and the greater anti-correlation between the two networks suggests excessive rivalry between the networks. Increased deactivation of specific default-network regions is associated with the positive symptoms of schizophrenia.
However, there was controversy and conflicting findings over whether post-mortem findings resulted from chronic antipsychotic treatment. Studies using SPET and PET methods in drug naive patients have generally failed to find any difference in dopamine D2 receptor density compared to controls. Recent findings from meta-analyses suggest that there may be a small elevation in dopamine D2 receptors in drug-free patients with schizophrenia, but the degree of overlap between patients and controls makes it unlikely that this is clinically meaningful. In addition, newer antipsychotic medication (called atypical antipsychotic medication) can be as potent as older medication (called typical antipsychotic medication) while also affecting serotonin function and having somewhat less of a dopamine blocking effect. In addition, dopamine pathway dysfunction has not been reliably shown to correlate with symptom onset or severity. Giving a more precise explanation of this discrepancy involves the monomer and dimer ratio, Dr Philip Seeman has said: "In schizophrenia, therefore, the density of [11C]methylspiperone sites rises, reflecting an increase in monomers, while the density of [11C]raclopride sites remains the same, indicating that the total population of D2 monomers and dimers does not change."
It is still thought that dopamine mesolimbic pathways may be hyperactive, resulting in hyperstimulation of D2 receptors and positive symptoms. There is also growing evidence that, conversely, mesocortical pathway dopamine projections to the prefrontal cortex might be hypoactive (underactive), resulting in hypostimulation of D1 receptors, which may be related to negative symptoms and cognitive impairment. The overactivity and underactivity in these different regions may be linked, and may not be due to a primary dysfunction of dopamine systems but to more general neurodevelopmental issues that precede them. Increased dopamine sensitivity may be a common final pathway.
Another reliable finding, repeatedly found, is that there is a some sixfold excess of binding sites insensitive to a certain testing agent (raclopride)Dr Seeman later said this increase was probably due to the increase in d2 monomers. Such an increase in monomers, occurs via the cooperativity mechanism which is responsible for d2high and d2low, the supersensitive and lowsensitivity states of the d2 dopamine receptor
Another one of Philip Seeman's findings was that the dopamine D2 receptor protein looked abnormal in schizophrenia. Proteins change states by flexing. The activating of the protein by folding could be permanent or fluctuating, just like the courses of patients' illnesses waxes and wanes. Increased folding of a protein leads to increased risk of 'additional fragments' forming The schizophrenic d2 receptor has a unique additional fragment when digested by papain in the test-tube in the FASEB experiment above, but none of the controls exhibited the same fragment. The D2 receptor in schizophrenia are thus in a highly active state as found by Philip Seeman et al.
There is evidence of irregular cellular metabolism and oxidative stress in the prefrontal cortex in schizophrenia, involving increased glucose demand and/or cellular hypoxia.
Mutations in the gene for brain-derived neurotrophic factor (BDNF) have been reported to be a risk factor for the disease.
Particular focus has been placed upon the function of dopamine in the mesolimbic pathway of the brain. This focus largely resulted from the accidental finding that a drug group which blocks dopamine function, known as the phenothiazines, could reducepsychotic symptoms. It is also supported by the fact that amphetamines, which triggers the release of dopamine may exacerbate the psychotic symptoms in schizophrenia. An influential theory, known as the Dopamine hypothesis of schizophrenia, proposed that excess activation of D2 receptors was the cause of (the positive symptoms of) schizophrenia. Although postulated for about 20 years based on the D2 blockade effect common to all antipsychotics, it was not until the mid-1990s that PET and SPET imaging studies provided supporting evidence. This theory is now thought to be overly simplistic as a complete explanation, partly because newer antipsychotic medication (called atypical antipsychotic medication) can be equally effective as older medication (called typical antipsychotic medication), but also affects serotonin function and may have slightly less of a dopamine blocking effect.
Interest has also focused on the neurotransmitter glutamate and the reduced function of the NMDA glutamate receptor in schizophrenia. This has largely been suggested by abnormally low levels of glutamate receptors found in postmortem brains of people previously diagnosed with schizophrenia and the discovery that the glutamate blocking drugs such as phencyclidine and ketamine can mimic the symptoms and cognitive problems associated with the condition. The fact that reduced glutamate function is linked to poor performance on tests requiring frontal lobe and hippocampal function and that glutamate can affect dopamine function, all of which have been implicated in schizophrenia, have suggested an important mediating (and possibly causal) role of glutamate pathways in schizophrenia. Positive symptoms fail however to respond to glutamatergic medication.
There have also been findings of differences in the size and structure of certain brain areas in schizophrenia. A 2006 metaanlaysis of MRI studies found that whole brain and hippocampal volume are reduced and that ventricular volume is increased in patients with a first psychotic episode relative to healthy controls. The average volumetric changes in these studies are however close to the limit of detection by MRI methods, so it remains to be determined whether schizophrenia is a neurodegenerative process that begins at about the time of symptom onset, or whether it is better characterised as a neurodevelopmental process that produces abnormal brain volumes at an early age. In first episode psychosis typical antipsychotics like haloperidol were associated with significant reductions in gray matter volume, whereas atypical antipsychotics likeolanzapine were not. Studies in non-human primates found gray and white matter reductions for both typical and atypical antipsychotics.
A 2009 meta-analysis of diffusion tensor imaging studies identified two consistent locations of fractional anisotropy reduction in schizophrenia. One region, in the left frontal lobe, is traversed by white matter tracts interconnecting the frontal lobe,thalamus and cingulate gyrus; the second region in the temporal lobe, is traversed by white matter tracts interconnecting the frontal lobe, insula, hippocampus–amygdala, temporal and occipital lobe. The authors suggest that two networks of white matter tracts may be affected in schizophrenia, with the potential for "disconnection" of the gray matter regions which they link. During fMRI studies, greater connectivity in thebrain's default network and task-positive network has been observed in schizophrenic patients, and may reflect excessive orientation of attention to introspection and to extrospection, respectively. The greater anti-correlation between the two networks suggests excessive rivalry between the networks.
Standardized criteria
The most widely used standardized criteria for diagnosing schizophrenia come from the American Psychiatric Association's Diagnostic and Statistical Manual of Mental Disorders, version DSM-IV-TR, and the World Health Organization's International Statistical Classification of Diseases and Related Health Problems, the ICD-10. The latter criteria are typically used in European countries, while the DSM criteria are used in the United States and the rest of the world, as well as prevailing in research studies. The ICD-10 criteria put more emphasis on Schneiderian first-rank symptoms, although, in practice, agreement between the two systems is high.According to the revised fourth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV-TR), to be diagnosed with schizophrenia, three diagnostic criteria must be met:
- Characteristic symptoms: Two or more of the following, each present for much of the time during a one-month period (or less, if symptoms remitted with treatment).
- Delusions
- Hallucinations
- Disorganized speech, which is a manifestation of formal thought disorder
- Grossly disorganized behavior (e.g. dressing inappropriately, crying frequently) or catatonic behavior
- Negative symptoms - affective flattening (lack or decline in emotional response), alogia (lack or decline in speech), or avolition (lack or decline in motivation)
- If the delusions are judged to be bizarre, or hallucinations consist of hearing one voice participating in a running commentary of the patient's actions or of hearing two or more voices conversing with each other, only that symptom is required above. The speech disorganization criterion is only met if it is severe enough to substantially impair communication.
- Social/occupational dysfunction: For a significant portion of the time since the onset of the disturbance, one or more major areas of functioning such as work, interpersonal relations, or self-care, are markedly below the level achieved prior to the onset.
- Duration: Continuous signs of the disturbance persist for at least six months. This six-month period must include at least one month of symptoms (or less, if symptoms remitted with treatment).
Confusion with other conditions
Psychotic symptoms may be present with several other psychiatric illnesses, includingbipolar disorder, borderline personality disorder, schizoaffective disorder, drug intoxication, either intoxicated or abstinent drug-induced psychosis, and schizophreniform disorder. Schizophrenia is complicated with obsessive-compulsive disorder (OCD) considerably more often than could be explained by pure chance, although it can be difficult to distinguish compulsions that represent OCD from the delusions characteristic of the schizophrenia.A more general medical and neurological examination may be needed to rule out medical illnesses which may rarely produce psychotic schizophrenia-like symptoms, such as metabolic disturbance, systemic infection, syphilis, HIV infection, epilepsy, and brainlesions. It may be necessary to rule out a delirium, which can be distinguished by visual hallucinations, acute onset and fluctuating level of consciousness, and indicates an underlying medical illness. Investigations are not generally repeated for relapse unless there is a specific medical indication or possible adverse effects from antipsychotic medication.
"Schizophrenia" does not mean dual personality, despite the etymology of the word (Greek σχίζω = "I split").
Subtypes
The DSM-IV-TR contains five sub-classifications of schizophrenia.- Paranoid type: Where delusions and hallucinations are present but thought disorder, disorganized behavior, and affective flattening are absent. (DSM code 295.3/ICD code F20.0)
- Disorganized type: Named hebephrenic schizophrenia in the ICD. Where thought disorder and flat affect are present together. (DSM code 295.1/ICD code F20.1)
- Catatonic type: The subject may be almost immobile or exhibit agitated, purposeless movement. Symptoms can include catatonic stupor and waxy flexibility. (DSM code 295.2/ICD code F20.2)
- Undifferentiated type: Psychotic symptoms are present but the criteria for paranoid, disorganized, or catatonic types have not been met. (DSM code 295.9/ICD code F20.3)
- Residual type: Where positive symptoms are present at a low intensity only. (DSM code 295.6/ICD code F20.5)
- Post-schizophrenic depression: A depressive episode arising in the aftermath of a schizophrenic illness where some low-level schizophrenic symptoms may still be present. (ICD code F20.4)
- Simple schizophrenia: Insidious and progressive development of prominent negative symptoms with no history of psychotic episodes. (ICD code F20.6)
Controversies and Research Directions
Part of a larger controversy over biopsychiatry, the validity of schizophrenia as a diagnostic entity has been criticised by number of psychologists as lacking in scientific validity and diagnostic reliability. In 2006, a group of patients and mental health professionals from the UK, under the banner of Campaign for Abolition of the Schizophrenia Label, argued for a rejection of the diagnosis of schizophrenia based on its heterogeneity and associated stigma, and called for the adoption of a bio-psychosocial model. Other UK psychiatrists opposed the move arguing that the term schizophrenia is a useful, even if provisional concept.The discrete category of schizophrenia used in the DSM has also been criticized. As with other psychiatric disorders, some psychiatrists have suggested that the diagnosis would be better addressed as individual dimensions along which everyone varies, such that there is a spectrum or continuum rather than a cut-off between normal and ill. This approach appears consistent with research on schizotypy, and with a relatively high prevalence of psychotic experiences, mostly non-distressing delusional beliefs, among the general public. In concordance with this observation, psychologist Edgar Jones, and psychiatrists Tony David and Nassir Ghaemi, surveying the existing literature on delusions, pointed out that the consistency and completeness of the definition ofdelusion have been found wanting by many; delusions are neither necessarily fixed, nor false, nor involve the presence of incontrovertible evidence.
Nancy Andreasen, a leading figure in schizophrenia research, has criticized the current DSM-IV and ICD-10 criteria for sacrificing validity for the sake of improving diagnostic reliability. She argues that overemphasis on psychosis in the diagnostic criteria, while improving diagnostic reliability, ignores more fundamental cognitive impairments that are harder to assess due to large variations in presentation. This view is supported by other psychiatrists. In the same vein, Ming Tsuang and colleagues argue that psychotic symptoms may be a common end-state in a variety of disorders, including schizophrenia, rather than a reflection of the specific etiology of schizophrenia, and warn that there is little basis for regarding DSM’s operational definition as the "true" construct of schizophrenia. Neuropsychologist Michael Foster Green went further in suggesting the presence of specific neurocognitive deficits may be used to construct phenotypes that are alternatives to those that are purely symptom-based. These deficits take the form of a reduction or impairment in basic psychological functions such as memory, attention, executive function and problem solving.
The exclusion of affective components from the criteria for schizophrenia, despite their ubiquity in clinical settings, has also become a bone of contention. This exclusion in the DSM has resulted in a "rather convoluted" separate disorder - schizoaffective disorder. Citing poor interrater reliability, some psychiatrists have totally contested the concept of schizoaffective disorder as a separate entity. The categorical distinction between mood disorders and schizophrenia, known as the Kraepelinian dichotomy, has also been challenged by data from genetic epidemiology.
Schizophrenia Neural Processes
Structural
Studies have tended to show various subtle average differences in the volume of certain areas of brain structure between people with and without diagnoses ofschizophrenia, although it has become increasingly clear that there is no single pathological neuropsychological or structural neuroanatomic profile, due partly to heterogeneity within the disorder. The most consistent volumetric findings are (first-onset patient vs control group averages), slightly less grey matter volume and slightly increased ventricular volume in certain areas of the brain. The two findings are thought to be linked. Although the differences are found in first-episode cases, grey matter volumes are partly a result of life experiences, drugs and malnutrition etc, so the exact role in the disorder is unclear. In addition, ventricle volumes are amongst the mostly highly variable and environmentally-influenced aspects of brain structure, and the percentage difference in group averages in schizophrenia studies has been described as "not a very profound difference in the context of normal variation." A slightly smaller than average whole-brain volume has also been also been found, and slightly smaller hippocampal volume in terms of group averages. These differences may be present from birth or develop later, and there is substantial variation between individuals.Most schizophrenia studies have found average reduced volume of the left medial temporal lobe and left superior temporal gyrus, and half of studies have revealed deficits in certain areas of the frontal gyrus, parahippocampal gyrus and temporal gyrus. However, at variance with some findings in individuals with chronic schizophrenia (where use of antipsychotics and other factors may have a confounding effect), significant group differences of temporal lobe and amygdala volumes are not shown in first-episode patients on average. The neurobiological abnormalities are so varied that no single abnormality is observed across the entire group of people with DSM-IV–defined schizophrenia. In addition, it remains unclear whether the structural differences are unique to schizophrenia or cut across the traditional diagnostic boundaries between schizophrenia and affective disorders - though perhaps being unique to conditions withpsychotic features.
Studies of the rare childhood-onset schizophrenia (before age 13) indicate a greater-than-normal loss of grey matter over several years, progressing from the back of the brain to the front, levelling out in early adulthood. Such a pattern of "pruning" occurs as part of normal brain development but appears to be exaggerated in childhood-onset psychotic diagnoses, particularly schizophrenia. Abnormalities in the volume of the ventricles or frontal lobes have also been found in several studies but not in others. Volume changes are most likely glial and vascular rather than purely neuronal, and reduction in grey matter may primarily reflect a reduction of neuropil rather than a deficit in the total number of neurons. Other studies, especially some computational studies, have shown that a reduction in the number of neurons can cause psychotic symptoms. Studies to date have been based on small numbers of the most severe and treatment-resistant patients taking antipsychotics.
Functional
Some studies using neuropsychological tests and brain imaging technologies such as fMRI and PET to examine functional differences in brain activity have shown that differences seem to most commonly occur in the frontal lobes, hippocampus, and temporal lobes. Abnormalities of the kind shown are linked to the same neurocognitive deficits often associated with schizophrenia, particularly in areas of memory, attention, problem solving, executive function, and social cognition. Observations of the frontal lobe in patients with schizophrenia are inconsistent: While many studies have found abnormalities, others have found no or only a statistically insignificant difference. Data from a PET study suggests that the less the frontal lobes are activated during a working memory task, the greater the increase in abnormal dopamine activity in the striatum, thought to be related to the neurocognitive deficits in schizophrenia.Electroencephalograph (EEG) recordings of persons with schizophrenia performing perception oriented tasks showed an absence of gamma band activity in the brain, indicating weak integration of critical neural networks in the brain. Those who experienced intense hallucinations, delusions and disorganized thinking showed the lowest frequency synchronization. None of the drugs taken by the persons scanned had moved neural synchrony back into the gamma frequency range. Gamma band and working memory alterations may be related to alterations in interneurons that produce the neurotransmitter GABA.
Atypical connectivity in the default network and other resting-state networks in the brain has been observed in schizophrenic patients. The greater connectivity in the default network and the task-positive network may reflect excessive orientation of attention to introspection and to extrospection, respectively, and the greater anti-correlation between the two networks suggests excessive rivalry between the networks. Increased deactivation of specific default-network regions is associated with the positive symptoms of schizophrenia.
Dopamine
Particular focus has been placed upon the function of dopamine in the mesolimbic pathway of the brain. This focus largely resulted from the accidental finding that a drug group which blocks dopamine function, known as the phenothiazines, could reduce psychotic symptoms. An influential theory, known as the "dopamine hypothesis of schizophrenia", proposed that a malfunction involving dopamine pathways was therefore the cause of (the positive symptoms of) schizophrenia. Evidence for this theory includes findings that the potency of many antipsychotics is correlated with their affinity todopamine D2 receptors; and the exacerbatory effects of a dopamine agonist (amphetamine) and a dopamine beta hydroxylase inhibitor (disulfiram) on schizophrenia; and post-mortem studies initially suggested increased density of dopamine D2 receptors in the striatum. Such high levels of D[2] receptors intensify brain signals in schizophrenia and causes positive symptoms such as hallucinations and paranoia. Impaired glutamate (a neurotransmitter which directs neuron to pass along an impulse) activity appears to be another source of schizophrenia symptoms.However, there was controversy and conflicting findings over whether post-mortem findings resulted from chronic antipsychotic treatment. Studies using SPET and PET methods in drug naive patients have generally failed to find any difference in dopamine D2 receptor density compared to controls. Recent findings from meta-analyses suggest that there may be a small elevation in dopamine D2 receptors in drug-free patients with schizophrenia, but the degree of overlap between patients and controls makes it unlikely that this is clinically meaningful. In addition, newer antipsychotic medication (called atypical antipsychotic medication) can be as potent as older medication (called typical antipsychotic medication) while also affecting serotonin function and having somewhat less of a dopamine blocking effect. In addition, dopamine pathway dysfunction has not been reliably shown to correlate with symptom onset or severity. Giving a more precise explanation of this discrepancy involves the monomer and dimer ratio, Dr Philip Seeman has said: "In schizophrenia, therefore, the density of [11C]methylspiperone sites rises, reflecting an increase in monomers, while the density of [11C]raclopride sites remains the same, indicating that the total population of D2 monomers and dimers does not change."
It is still thought that dopamine mesolimbic pathways may be hyperactive, resulting in hyperstimulation of D2 receptors and positive symptoms. There is also growing evidence that, conversely, mesocortical pathway dopamine projections to the prefrontal cortex might be hypoactive (underactive), resulting in hypostimulation of D1 receptors, which may be related to negative symptoms and cognitive impairment. The overactivity and underactivity in these different regions may be linked, and may not be due to a primary dysfunction of dopamine systems but to more general neurodevelopmental issues that precede them. Increased dopamine sensitivity may be a common final pathway.
Another reliable finding, repeatedly found, is that there is a some sixfold excess of binding sites insensitive to a certain testing agent (raclopride)Dr Seeman later said this increase was probably due to the increase in d2 monomers. Such an increase in monomers, occurs via the cooperativity mechanism which is responsible for d2high and d2low, the supersensitive and lowsensitivity states of the d2 dopamine receptor
Another one of Philip Seeman's findings was that the dopamine D2 receptor protein looked abnormal in schizophrenia. Proteins change states by flexing. The activating of the protein by folding could be permanent or fluctuating, just like the courses of patients' illnesses waxes and wanes. Increased folding of a protein leads to increased risk of 'additional fragments' forming The schizophrenic d2 receptor has a unique additional fragment when digested by papain in the test-tube in the FASEB experiment above, but none of the controls exhibited the same fragment. The D2 receptor in schizophrenia are thus in a highly active state as found by Philip Seeman et al.
Glutamate
Interest has also focused on the neurotransmitter glutamate and the reduced function of the NMDA glutamate receptor in schizophrenia. This has largely been suggested by abnormally low levels of glutamate receptors found in postmortem brains of people previously diagnosed with schizophrenia and the discovery that the glutamate blocking drugs such as phencyclidine and ketamine can mimic the symptoms and cognitive problems associated with the condition. The fact that reduced glutamate function is linked to poor performance on tests requiring frontal lobe and hippocampal function and that glutamate can affect dopamine function, all of which have been implicated inschizophrenia, have suggested an important mediating (and possibly causal) role of glutamate pathways in schizophrenia. Further support of this theory has come from preliminary trials suggesting the efficacy of coagonists at the NMDA receptor complex in reducing some of the positive symptoms of schizophrenia.Other
Dyregulation of neural calcium homeostasis has been hypothesized to be a link between the glutamate and dopaminergic abnormalities and some small studies have indicated that calcium channel blocking agents can lead to improvements on some measures in schizophrenia with tardive dyskinesia.There is evidence of irregular cellular metabolism and oxidative stress in the prefrontal cortex in schizophrenia, involving increased glucose demand and/or cellular hypoxia.
Mutations in the gene for brain-derived neurotrophic factor (BDNF) have been reported to be a risk factor for the disease.
Schizophrenia Mechanisms
Psychological
A number of non-causal psychological mechanisms have been implicated in the development and maintenance of schizophrenia. Cognitive biases that have been identified in those with a diagnosis or those at risk, especially when under stress or in confusing situations, include excessive attention to potential threats, jumping to conclusions, making external attributions, impaired reasoning about social situations and mental states, difficulty distinguishing inner speech from speech from an external source, and difficulties with early visual processing and maintaining concentration. Some cognitive features may reflect global neurocognitive deficits in memory, attention, problem-solving, executive function or social cognition, while others may be related to particular issues and experiences. Despite a common appearance of "blunted affect", recent findings indicate that many individuals diagnosed with schizophrenia are highly emotionally responsive, particularly to stressful or negative stimuli, and that such sensitivity may cause vulnerability to symptoms or to the disorder. Some evidence suggests that the content of delusional beliefs and psychotic experiences can reflect emotional causes of the disorder, and that how a person interprets such experiences can influence symptomatology. The use of "safety behaviors" to avoid imagined threats may contribute to the chronicity of delusions. Further evidence for the role of psychological mechanisms comes from the effects of therapies on symptoms of schizophrenia.Neural
Studies using neuropsychological tests and brain imaging technologies such as fMRI and PET to examine functional differences in brain activity have shown that differences seem to most commonly occur in the frontal lobes, hippocampus and temporal lobes. These differences have been linked to the neurocognitive deficits often associated with schizophrenia.Particular focus has been placed upon the function of dopamine in the mesolimbic pathway of the brain. This focus largely resulted from the accidental finding that a drug group which blocks dopamine function, known as the phenothiazines, could reducepsychotic symptoms. It is also supported by the fact that amphetamines, which triggers the release of dopamine may exacerbate the psychotic symptoms in schizophrenia. An influential theory, known as the Dopamine hypothesis of schizophrenia, proposed that excess activation of D2 receptors was the cause of (the positive symptoms of) schizophrenia. Although postulated for about 20 years based on the D2 blockade effect common to all antipsychotics, it was not until the mid-1990s that PET and SPET imaging studies provided supporting evidence. This theory is now thought to be overly simplistic as a complete explanation, partly because newer antipsychotic medication (called atypical antipsychotic medication) can be equally effective as older medication (called typical antipsychotic medication), but also affects serotonin function and may have slightly less of a dopamine blocking effect.
Interest has also focused on the neurotransmitter glutamate and the reduced function of the NMDA glutamate receptor in schizophrenia. This has largely been suggested by abnormally low levels of glutamate receptors found in postmortem brains of people previously diagnosed with schizophrenia and the discovery that the glutamate blocking drugs such as phencyclidine and ketamine can mimic the symptoms and cognitive problems associated with the condition. The fact that reduced glutamate function is linked to poor performance on tests requiring frontal lobe and hippocampal function and that glutamate can affect dopamine function, all of which have been implicated in schizophrenia, have suggested an important mediating (and possibly causal) role of glutamate pathways in schizophrenia. Positive symptoms fail however to respond to glutamatergic medication.
There have also been findings of differences in the size and structure of certain brain areas in schizophrenia. A 2006 metaanlaysis of MRI studies found that whole brain and hippocampal volume are reduced and that ventricular volume is increased in patients with a first psychotic episode relative to healthy controls. The average volumetric changes in these studies are however close to the limit of detection by MRI methods, so it remains to be determined whether schizophrenia is a neurodegenerative process that begins at about the time of symptom onset, or whether it is better characterised as a neurodevelopmental process that produces abnormal brain volumes at an early age. In first episode psychosis typical antipsychotics like haloperidol were associated with significant reductions in gray matter volume, whereas atypical antipsychotics likeolanzapine were not. Studies in non-human primates found gray and white matter reductions for both typical and atypical antipsychotics.
A 2009 meta-analysis of diffusion tensor imaging studies identified two consistent locations of fractional anisotropy reduction in schizophrenia. One region, in the left frontal lobe, is traversed by white matter tracts interconnecting the frontal lobe,thalamus and cingulate gyrus; the second region in the temporal lobe, is traversed by white matter tracts interconnecting the frontal lobe, insula, hippocampus–amygdala, temporal and occipital lobe. The authors suggest that two networks of white matter tracts may be affected in schizophrenia, with the potential for "disconnection" of the gray matter regions which they link. During fMRI studies, greater connectivity in thebrain's default network and task-positive network has been observed in schizophrenic patients, and may reflect excessive orientation of attention to introspection and to extrospection, respectively. The greater anti-correlation between the two networks suggests excessive rivalry between the networks.
Schizophrenia Screening, Prevention and Management
There are no reliable markers for the later development of schizophrenia although research is being conducted into how well a combination of genetic risk plus non-disabling psychosis-like experience predicts later diagnosis. People who fulfill the 'ultra high-risk mental state' criteria, that include a family history of schizophrenia plus the presence of transient or self-limiting psychotic experiences, have a 20–40% chance of being diagnosed with the condition after one year. The use of psychological treatments and medication has been found effective in reducing the chances of people who fulfill the 'high-risk' criteria from developing full-blown schizophrenia. However, the treatment of people who may never develop schizophrenia is controversial, in light of the side-effects of antipsychotic medication; particularly with respect to the potentially disfiguring tardive dyskinesia and the rare but potentially lethal neuroleptic malignant syndrome. The most widely used form of preventative health care for schizophrenia takes the form of public education campaigns that provide information on risk factors and early symptoms, with the aim to improve detection and provide treatment earlier for those experiencing delays. The new clinical approach early intervention in psychosis is a secondary prevention strategy to prevent further episodes and prevent the long term disability associated with schizophrenia.
The concept of a cure as such remains controversial, as there is no consensus on the definition, although some criteria for the remission of symptoms have recently been suggested. The effectiveness of schizophrenia treatment is often assessed using standardized methods, one of the most common being the Positive and Negative Syndrome Scale (PANSS). Management of symptoms and improving function is thought to be more achievable than a cure. Treatment was revolutionized in the mid-1950s with the development and introduction of chlorpromazine. A recovery model is increasingly adopted, emphasizing hope, empowerment and social inclusion.
Hospitalization may occur with severe episodes of schizophrenia. This can be voluntary or (if mental health legislation allows it) involuntary (called civil or involuntary commitment). Long-term inpatient stays are now less common due to deinstitutionalization, although can still occur. Following (or in lieu of) a hospital admission, support services available can include drop-in centers, visits from members of a community mental health team or Assertive Community Treatment team, supported employment and patient-led support groups.
In many non-Western societies, schizophrenia may only be treated with more informal, community-led methods. Multiple international surveys by the World Health Organization over several decades have indicated that the outcome for people diagnosed with schizophrenia in non-Western countries is on average better there than for people in the West. Many clinicians and researchers suspect the relative levels of social connectedness and acceptance are the difference, although further cross-cultural studies are seeking to clarify the findings.
The concept of a cure as such remains controversial, as there is no consensus on the definition, although some criteria for the remission of symptoms have recently been suggested. The effectiveness of schizophrenia treatment is often assessed using standardized methods, one of the most common being the Positive and Negative Syndrome Scale (PANSS). Management of symptoms and improving function is thought to be more achievable than a cure. Treatment was revolutionized in the mid-1950s with the development and introduction of chlorpromazine. A recovery model is increasingly adopted, emphasizing hope, empowerment and social inclusion.
Hospitalization may occur with severe episodes of schizophrenia. This can be voluntary or (if mental health legislation allows it) involuntary (called civil or involuntary commitment). Long-term inpatient stays are now less common due to deinstitutionalization, although can still occur. Following (or in lieu of) a hospital admission, support services available can include drop-in centers, visits from members of a community mental health team or Assertive Community Treatment team, supported employment and patient-led support groups.
In many non-Western societies, schizophrenia may only be treated with more informal, community-led methods. Multiple international surveys by the World Health Organization over several decades have indicated that the outcome for people diagnosed with schizophrenia in non-Western countries is on average better there than for people in the West. Many clinicians and researchers suspect the relative levels of social connectedness and acceptance are the difference, although further cross-cultural studies are seeking to clarify the findings.
Schizophrenia Medication
The first line psychiatric treatment for schizophrenia is antipsychotic medication. These can reduce the positive symptoms of psychosis. Most antipsychotics take around 7–14 days to have their main effect. Currently available antipsychotics fail however to significantly ameliorate the negative symptoms, and the improvements on cognition may be attributed to the practice effect.
The newer atypical antipsychotic drugs are usually preferred for initial treatment over the older typical antipsychotic, although they are expensive and are more likely to induce weight gain and obesity-related diseases. In 2008, results from a major randomized trial sponsored by the US National Institute of Mental Health (Clinical Antipsychotic Trials of Intervention Effectiveness, or CATIE) found that a representative first-generation antipsychotic, perphenazine, was as effective as and more cost-effective than several newer drugs (olanzapine, perphenazine, quetiapine, risperidone, or ziprasidone) taken for up to 18 months. The atypical antipsychotic which patients were willing to continue for the longest, olanzapine, was associated with considerable weight gain and risk of metabolic syndrome. Clozapine was most effective for people with a poor response to other drugs, but it had troublesome side effects. Because the trial excluded patients with tardive dyskinesia, its relevance to these people is unclear.
The two classes of antipsychotics are generally thought equally effective for the treatment of the positive symptoms. Some researchers have suggested that the atypicals offer additional benefit for the negative symptoms and cognitive deficits associated with schizophrenia, although the clinical significance of these effects has yet to be established.
Because of their reportedly lower risk of side effects that affect mobility, atypical antipsychotics have been first-line treatment for early-onset schizophrenia for many years before certain drugs in this class were approved by the Food and Drug Administration for use in children and teenagers with schizophrenia. This advantage comes at the cost of an increased risk of metabolic syndrome and obesity, which is of concern in the context of long-term use begun at an early age. Especially in the case of children and teenagers who have schizophrenia, medication should be used in combination with individual therapy and family-based interventions.
Recent reviews have refuted the claim that atypical antipsychotics have fewer extrapyramidal side effects than typical antipsychotics, especially when the latter are used in low doses or when low potency antipsychotics are chosen.
Prolactin elevations have been reported in women with schizophrenia taking atypical antipsychotics. It remains unclear whether the newer antipsychotics reduce the chances of developing neuroleptic malignant syndrome, a rare but serious and potentially fatal neurological disorder most often caused by an adverse reaction to neuroleptic or antipsychotic drugs.
Response of symptoms to medication is variable: treatment-resistant schizophrenia is a term used for the failure of symptoms to respond satisfactorily to at least two different antipsychotics. Patients in this category may be prescribed clozapine, a medication of superior effectiveness but several potentially lethal side effects including agranulocytosis and myocarditis. Clozapine may have the additional benefit of reducing propensity for substance abuse in schizophrenic patients. For other patients who are unwilling or unable to take medication regularly, long-acting depot preparations of antipsychotics may be given every two weeks to achieve control. The United States and Australia are two countries with laws allowing the forced administration of this type of medication on those who refuse but are otherwise stable and living in the community. At least one study suggested that in the longer-term some individuals may do better not taking antipsychotics.
A 2003 review of four randomized controlled trials of EPA (an omega-3 fatty acid) vs. placebo as adjunctive treatment for schizophrenia found that two of the trials detected a significant improvement on positive and negative symptoms, and suggested that EPA may be an effective adjunct to antipsychotics. The most recent meta-analysis (2006) failed however to find a significant effect. A 2007 review found that studies of omega-3 fatty acids in schizophrenia, despite being mostly of high quality, have produced inconsistent results and small effect sizes of doubtful clinical significance.
 |
The two classes of antipsychotics are generally thought equally effective for the treatment of the positive symptoms. Some researchers have suggested that the atypicals offer additional benefit for the negative symptoms and cognitive deficits associated with schizophrenia, although the clinical significance of these effects has yet to be established.
Because of their reportedly lower risk of side effects that affect mobility, atypical antipsychotics have been first-line treatment for early-onset schizophrenia for many years before certain drugs in this class were approved by the Food and Drug Administration for use in children and teenagers with schizophrenia. This advantage comes at the cost of an increased risk of metabolic syndrome and obesity, which is of concern in the context of long-term use begun at an early age. Especially in the case of children and teenagers who have schizophrenia, medication should be used in combination with individual therapy and family-based interventions.
Recent reviews have refuted the claim that atypical antipsychotics have fewer extrapyramidal side effects than typical antipsychotics, especially when the latter are used in low doses or when low potency antipsychotics are chosen.
Prolactin elevations have been reported in women with schizophrenia taking atypical antipsychotics. It remains unclear whether the newer antipsychotics reduce the chances of developing neuroleptic malignant syndrome, a rare but serious and potentially fatal neurological disorder most often caused by an adverse reaction to neuroleptic or antipsychotic drugs.
Response of symptoms to medication is variable: treatment-resistant schizophrenia is a term used for the failure of symptoms to respond satisfactorily to at least two different antipsychotics. Patients in this category may be prescribed clozapine, a medication of superior effectiveness but several potentially lethal side effects including agranulocytosis and myocarditis. Clozapine may have the additional benefit of reducing propensity for substance abuse in schizophrenic patients. For other patients who are unwilling or unable to take medication regularly, long-acting depot preparations of antipsychotics may be given every two weeks to achieve control. The United States and Australia are two countries with laws allowing the forced administration of this type of medication on those who refuse but are otherwise stable and living in the community. At least one study suggested that in the longer-term some individuals may do better not taking antipsychotics.
A 2003 review of four randomized controlled trials of EPA (an omega-3 fatty acid) vs. placebo as adjunctive treatment for schizophrenia found that two of the trials detected a significant improvement on positive and negative symptoms, and suggested that EPA may be an effective adjunct to antipsychotics. The most recent meta-analysis (2006) failed however to find a significant effect. A 2007 review found that studies of omega-3 fatty acids in schizophrenia, despite being mostly of high quality, have produced inconsistent results and small effect sizes of doubtful clinical significance.
Schizophrenia Interventions
Psychotherapy is also widely recommended and used in the treatment of schizophrenia, although services may often be confined to pharmacotherapy because of reimbursement problems or lack of training.
Cognitive behavioral therapy (CBT) is used to target specific symptoms and improve related issues such as self-esteem, social functioning, and insight. Although the results of early trials were inconclusive as the therapy advanced from its initial applications in the mid 1990s, more recent reviews clearly show CBT is an effective treatment for thepsychotic symptoms of schizophrenia
Another approach is cognitive remediation therapy, a technique aimed at remediating the neurocognitive deficits sometimes present in schizophrenia. Based on techniques of neuropsychological rehabilitation, early evidence has shown it to be cognitively effective, with some improvements related to measurable changes in brain activation as measured by fMRI. A similar approach known as cognitive enhancement therapy, which focuses on social cognition as well as neurocognition, has shown efficacy.
Family therapy or education, which addresses the whole family system of an individual with a diagnosis of schizophrenia, has been consistently found to be beneficial, at least if the duration of intervention is longer-term. Aside from therapy, the impact of schizophrenia on families and the burden on carers has been recognized, with the increasing availability of self-help books on the subject. There is also some evidence for benefits from social skills training, although there have also been significant negative findings. Some studies have explored the possible benefits of music therapy and other creative therapies.
The Soteria model is alternative to inpatient hospital treatment using a minimal medication approach. It is described as a milieu-therapeutic recovery method, characterized by its founder as "the 24 hour a day application of interpersonal phenomenologic interventions by a nonprofessional staff, usually without neuroleptic drug treatment, in the context of a small, homelike, quiet, supportive, protective, and tolerant social environment." Although research evidence is limited, a 2008 systematic review found the programme equally as effective as treatment with medication in people diagnosed with first and second episode schizophrenia.
Service-user led movements have become integral to the recovery process in Europe and the United States; groups such as the Hearing Voices Network and the ParanoiaNetwork have developed a self-help approach that aims to provide support and assistance outside the traditional medical model adopted by mainstream psychiatry. By avoiding framing personal experience in terms of criteria for mental illness or mental health, they aim to destigmatize the experience and encourage individual responsibility and a positive self-image. Partnerships between hospitals and consumer-run groups are becoming more common, with services working toward remediating social withdrawal, building social skills and reducing rehospitalization.
A clinical study using strict recovery criteria (concurrent remission of positive and negative symptoms and adequate social and vocational functioning continuously for two years) found a recovery rate of 14% within the first five years. A 5-year community study found that 62% showed overall improvement on a composite measure of clinical and functional outcomes.
World Health Organization studies have noted that individuals diagnosed with schizophrenia have much better long-term outcomes in developing countries (India, Colombia and Nigeria) than in developed countries (United States, United Kingdom, Ireland, Denmark, Czech Republic, Slovakia, Japan, and Russia), despite antipsychotic drugs not being widely available.
Rates are not always comparable across studies because exact definitions of remission and recovery have not been widely established. A "Remission in Schizophrenia Working Group" has proposed standardized remission criteria involving "improvements in core signs and symptoms to the extent that any remaining symptoms are of such low intensity that they no longer interfere significantly with behavior and are below the threshold typically utilized in justifying an initial diagnosis of schizophrenia". Standardized recovery criteria have also been proposed by a number of different researchers, with the stated DSM definitions of a "complete return to premorbid levels of functioning” or "complete return to full functioning" seen as inadequate, impossible to measure, incompatible with the variability in how society defines normal psychosocial functioning, and contributing to self-fulfilling pessimism and stigma. Some mental health professionals may have quite different basic perceptions and concepts of recovery than individuals with the diagnosis, including those in the consumer/survivor movement. One notable limitation of nearly all the research criteria is failure to address the person's own evaluations and feelings about their life. Schizophrenia and recovery often involve a continuing loss of self-esteem, alienation from friends and family, interruption of school and career, and social stigma, "experiences that cannot just be reversed or forgotten". An increasingly influential model defines recovery as a process, similar to being "in recovery" from drug and alcohol problems, and emphasizes a personal journey involving factors such as hope, choice, empowerment, social inclusion and achievement.
There is a higher than average suicide rate associated with schizophrenia. This has been cited at 10%, but a more recent analysis of studies and statistics revises the estimate at 4.9%, most often occurring in the period following onset or first hospital admission. Several times more attempt suicide. There are a variety of reasons and risk factors.
The occurrence of psychosis in schizophrenia has sometimes been linked to a higher risk of violent acts. Findings on the specific role of delusions or hallucinations have been inconsistent, but have focused on delusional jealousy, perception of threat and command hallucinations. It has been proposed that a certain type of individual withschizophrenia may be most likely to offend, characterized by a history of educational difficulties, low IQ, conduct disorder, early-onset substance misuse and offending prior to diagnosis.
Individuals with a diagnosis of schizophrenia are often the victims of violent crime - at least 14 times more often than they are perpetrators. Another consistent finding is a link to substance misuse, particularly alcohol, among the minority who commit violent acts. Violence by or against individuals with schizophrenia typically occurs in the context of complex social interactions within a family setting, and is also an issue in clinical services and in the wider community.
Cognitive behavioral therapy (CBT) is used to target specific symptoms and improve related issues such as self-esteem, social functioning, and insight. Although the results of early trials were inconclusive as the therapy advanced from its initial applications in the mid 1990s, more recent reviews clearly show CBT is an effective treatment for thepsychotic symptoms of schizophrenia
Another approach is cognitive remediation therapy, a technique aimed at remediating the neurocognitive deficits sometimes present in schizophrenia. Based on techniques of neuropsychological rehabilitation, early evidence has shown it to be cognitively effective, with some improvements related to measurable changes in brain activation as measured by fMRI. A similar approach known as cognitive enhancement therapy, which focuses on social cognition as well as neurocognition, has shown efficacy.
Family therapy or education, which addresses the whole family system of an individual with a diagnosis of schizophrenia, has been consistently found to be beneficial, at least if the duration of intervention is longer-term. Aside from therapy, the impact of schizophrenia on families and the burden on carers has been recognized, with the increasing availability of self-help books on the subject. There is also some evidence for benefits from social skills training, although there have also been significant negative findings. Some studies have explored the possible benefits of music therapy and other creative therapies.
The Soteria model is alternative to inpatient hospital treatment using a minimal medication approach. It is described as a milieu-therapeutic recovery method, characterized by its founder as "the 24 hour a day application of interpersonal phenomenologic interventions by a nonprofessional staff, usually without neuroleptic drug treatment, in the context of a small, homelike, quiet, supportive, protective, and tolerant social environment." Although research evidence is limited, a 2008 systematic review found the programme equally as effective as treatment with medication in people diagnosed with first and second episode schizophrenia.
Other
Electroconvulsive therapy is not considered a first line treatment but may be prescribed in cases where other treatments have failed. It is more effective where symptoms of catatonia are present, and is recommended for use under NICE guidelines in the UK for catatonia if previously effective, though there is no recommendation for use for schizophrenia otherwise. Psychosurgery has now become a rare procedure and is not a recommended treatment.Service-user led movements have become integral to the recovery process in Europe and the United States; groups such as the Hearing Voices Network and the ParanoiaNetwork have developed a self-help approach that aims to provide support and assistance outside the traditional medical model adopted by mainstream psychiatry. By avoiding framing personal experience in terms of criteria for mental illness or mental health, they aim to destigmatize the experience and encourage individual responsibility and a positive self-image. Partnerships between hospitals and consumer-run groups are becoming more common, with services working toward remediating social withdrawal, building social skills and reducing rehospitalization.
Alternative Treatments
Orthomolecular psychiatry considers schizophrenia to be a group of disorders, some of which can be treated with megadoses of nutrients, such as Niacin (vitamin B-3). Proponents of orthomolecular psychiatry claim that an adverse reaction to gluten is involved in the etiology of some cases. This theory - discussed by one author in three British journals in the 1970s - is unproven. A 2006 literature review suggests that gluten may be a factor for patients with celiac disease and for a subset of patients afflicted with schizophrenia, but that further study is needed to conclusively confirm such a link. In a 2004 Israeli study, anti-gluten antibodies were measured in 50 patients with schizophrenia and a matched control group. All antibody tests in both groups were negative leading to the conclusion that "it is unlikely that there is an association between gluten sensitivity and schizophrenia". Some researchers suggest that dietary and nutritional treatments may hold promise in the treatment of schizophrenia.Schizophrenia Prognosis
Course
Coordinated by the World Health Organization and published in 2001, The International Study of Schizophrenia (ISoS) was a long-term follow-up study of 1633 individuals diagnosed with schizophrenia around the world. The striking difference in course and outcomes was noted; a half of those available for follow-up had a favourable outcome and 16% had a delayed recovery after an early unremitting course. More usually, the course in the first two years predicted the long-term course. Early social intervention was also related to a better outcome. The findings were held as important in moving patients, carers and clinicians away from the prevalent belief of the chronic nature of the condition. A review of major longitudinal studies in North America noted this variation in outcomes, although outcome was on average worse than for otherpsychotic and psychiatric disorders. A moderate number of patients with schizophrenia were seen to remit and remain well; the review raised the question that some may not require maintenance medication.A clinical study using strict recovery criteria (concurrent remission of positive and negative symptoms and adequate social and vocational functioning continuously for two years) found a recovery rate of 14% within the first five years. A 5-year community study found that 62% showed overall improvement on a composite measure of clinical and functional outcomes.
 |
Rates are not always comparable across studies because exact definitions of remission and recovery have not been widely established. A "Remission in Schizophrenia Working Group" has proposed standardized remission criteria involving "improvements in core signs and symptoms to the extent that any remaining symptoms are of such low intensity that they no longer interfere significantly with behavior and are below the threshold typically utilized in justifying an initial diagnosis of schizophrenia". Standardized recovery criteria have also been proposed by a number of different researchers, with the stated DSM definitions of a "complete return to premorbid levels of functioning” or "complete return to full functioning" seen as inadequate, impossible to measure, incompatible with the variability in how society defines normal psychosocial functioning, and contributing to self-fulfilling pessimism and stigma. Some mental health professionals may have quite different basic perceptions and concepts of recovery than individuals with the diagnosis, including those in the consumer/survivor movement. One notable limitation of nearly all the research criteria is failure to address the person's own evaluations and feelings about their life. Schizophrenia and recovery often involve a continuing loss of self-esteem, alienation from friends and family, interruption of school and career, and social stigma, "experiences that cannot just be reversed or forgotten". An increasingly influential model defines recovery as a process, similar to being "in recovery" from drug and alcohol problems, and emphasizes a personal journey involving factors such as hope, choice, empowerment, social inclusion and achievement.
Predictors
Several factors have been associated with a better overall prognosis: Being female, rapid (vs. insidious) onset of symptoms, older age of first episode, predominantly positive (rather than negative) symptoms, presence of mood symptoms, and good pre-illness functioning. The strengths and internal resources of the individual concerned, such as determination or psychological resilience, have also been associated with better prognosis. The attitude and level of support from people in the individual's life can have a significant impact; research framed in terms of the negative aspects of this - the level of critical comments, hostility, and intrusive or controlling attitudes, termed high 'Expressed emotion' - has consistently indicated links to relapse. Most research on predictive factors is correlational in nature, however, and a clear cause-and-effect relationship is often difficult to establish.Mortality
In a study of over 168,000 Swedish citizens undergoing psychiatric treatment, schizophrenia was associated with an average life expectancy of approximately 80–85% of that of the general population; women were found to have a slightly better life expectancy than men, and a diagnosis of schizophrenia was associated with an overall better life expectancy than substance abuse, personality disorder, heart attack andstroke. Other identified factors include smoking, poor diet, little exercise and the negative health effects of psychiatric drugs.There is a higher than average suicide rate associated with schizophrenia. This has been cited at 10%, but a more recent analysis of studies and statistics revises the estimate at 4.9%, most often occurring in the period following onset or first hospital admission. Several times more attempt suicide. There are a variety of reasons and risk factors.
Violence
The relationship between violent acts and schizophrenia is a contentious topic. Current research indicates that the percentage of people with schizophrenia who commit violent acts is higher than the percentage of people without any disorder, but lower than is found for disorders such as alcoholism, and the difference is reduced or not found in same-neighbourhood comparisons when related factors are taken into account, notably sociodemographic variables and substance misuse. Studies have indicated that 5% to 10% of those charged with murder in Western countries have a schizophrenia spectrum disorder.The occurrence of psychosis in schizophrenia has sometimes been linked to a higher risk of violent acts. Findings on the specific role of delusions or hallucinations have been inconsistent, but have focused on delusional jealousy, perception of threat and command hallucinations. It has been proposed that a certain type of individual withschizophrenia may be most likely to offend, characterized by a history of educational difficulties, low IQ, conduct disorder, early-onset substance misuse and offending prior to diagnosis.
Individuals with a diagnosis of schizophrenia are often the victims of violent crime - at least 14 times more often than they are perpetrators. Another consistent finding is a link to substance misuse, particularly alcohol, among the minority who commit violent acts. Violence by or against individuals with schizophrenia typically occurs in the context of complex social interactions within a family setting, and is also an issue in clinical services and in the wider community.
Clinical Trials
NIMH supports research studies on mental health and disorders. See also: A Participant's Guide to Mental Health Clinical Research.
Participate, refer a patient or learn about results of studies inClinicalTrials.gov, the NIH/National Library of Medicine's registry of federally and privately funded clinical trials for all disease.
Find NIH-funded studies currently recruiting participants withschizophrenia.
.jpg)
No comments:
Post a Comment
Note: Only a member of this blog may post a comment.